The Case of the Shih Tzu That Couldn’t Pee

What’s Your Diagnosis?
This is Chang Lu, a 10-year-old Shih Tzu. Chang Lu visited Medical District Veterinary Clinic in December with a history of straining to urinate, increased frequency of urination, and bloody urine.
During her exam she was trying to urinary every few minutes and was producing small, blood-tinged urine droplets each time. Initial diagnostics included urinalysis and X-rays. Her urine revealed significant bacteria and an overabundance of white blood cells. Below are her X-rays.
What is your diagnosis?
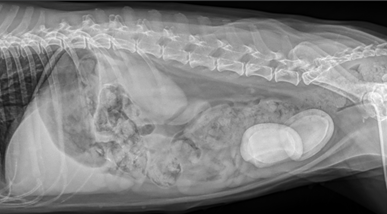
If you diagnosed Chang Lu with urinary tract infection and urinary bladder stones (urolithiasis), then you are correct. The large egg-shaped structures should not be there. Those are large urinary calculi (stones). Below I have notated the X-ray to point out various organs.
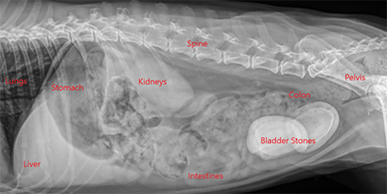
Urolithiasis (urinary bladder stones) are common in both dogs and cats. In people, most urinary stones originate in the kidneys, but in animals, more than 90% originate in the bladder, or lower urinary tract.
Urolithiasis (Urinary Bladder Stones)
Many factors, including genetic predisposition, can lead to bladder stones. Smaller breed dogs are at higher risk of developing urinary calculi (stones). Other predisposing factor include urinary tract infections, urine pH, urine mineral composition, and urine concentration.
When we see patients exhibiting the signs Chang Lu came in with (inappropriate urination, bloody urine, straining to urinate, increased frequency of urination), the most likely cause in dogs is a urinary tract infection and in cats is idiopathic (stress-induced) cystitis. In both species, however, it is important to rule out bladder stones, especially if urinary issues have been an ongoing problem for the pet.
To diagnose urinary bladder stones, veterinarians need to look inside the abdomen using X-rays and/or ultrasound. Seeing these stones is easier on X-rays than with ultrasound, and the number of stones can be more easily counted. Unfortunately, not all stones show up on X-rays, so ultrasound is needed to diagnose the non-radiopaque stones. Luckily, those that can’t be seen on X-ray are the much less common than those that can.
Treatment for Urinary Bladder Stones
Once stones have been diagnosed, treatment usually consists of a cystotomy (surgical removal of the stones) and treating the infection, if one is present. In some cases, prescription diets can be used to try to dissolve the stones. I personally have had great success with dissolution of stones in cats but very little to no success of dissolving stones with diet in dogs.
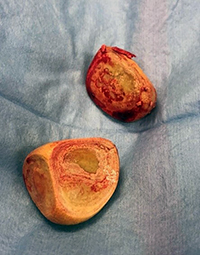
Chang Lu underwent a cystotomy, and two large stones were removed from her urinary bladder (see photo). At the time of surgery, we took a bacterial culture of her bladder, and the results showed that she had a resistant bacterial urinary tract infection. A resistant bacterial infection means the bacteria present in her bladder was resistant to most antibiotics, including the one she was initially prescribed. She was prescribed a new antibiotic in hopes the infection would be cleared.
How to Prevent Urinary Bladder Stones
Once stones have been diagnosed, it is very important to identify the type of stone to understand steps that can be taken to help prevent re-occurrence. After any cystotomy, the stones are sent to the University of Minnesota Urolith Laboratory, where the stones are evaluated. Knowing the mineral composition of the stone helps veterinarians determine the best way to prevent stones in the future. In many cases, pets are started on a long-term prescription diet to help alter their urine pH, encourage urine dilution, and limit the mineral components of the diet that lead to stone formation.
Chang Lu’s stones were determined to be 100% struvite stones, most likely secondary to her resistant bacterial infection. After she finished the course of new antibiotics, her urine was re-cultured, and the infection was completely cleared. Moving forward we will be screening her urine for infection every 3 to 6 months. She has also been switched to a prescription food designed to keep new stones from forming. Chang Lu is currently doing great and all her clinical signs have resolved.
– Dr. Drew Sullivan
