Our Blog
How Do You Know What to Feed Your Dog?

As a veterinarian, I get asked quite a few questions, and a handful of them are in competition for the title of “least favorite question.”
What’s the best breed of dog? Why does tick prevention cost more than heartworm prevention? Do I really need that vaccine? Can you look at my dog’s poop? (This one is often accompanied by a photo.) Can you smell this?
And the one I get asked the most: What’s the best food that I can feed my dog?
For most of these questions there is no simple answer, but the one about the best diet may be the hardest to answer. There are so many pet food options and so little regulation of how pet food companies can make and market their diets.
So, what can you trust?
We at Medical District Veterinary Clinic want to facilitate our clients picking a diet that works for their pets and their family as a whole. That means we understand that the cost, type, and how often you feed your pet varies by family. With so many choices available, we often rely on AAFCO standards to know if the diet you select for your pet is adequate.
Who or What Is AAFCO?
AAFCO (which stands for Association of American Feed Control Officials) is a non-profit organization that has been guiding government officials for over 100 years in determining nutritional standards for all pet foods.
Here is their mission statement: AAFCO is a collaborative association that supports members and stakeholders and promotes a safe feed supply through unified system-based regulation, feed ingredients standards, and laboratory operations.
This organization ensures that a diet has the essential nutrients for your pet, with different standards for all types and life stages of pets. That means the AAFCO label will tell you what kind of animal this diet is appropriate for, from a growing puppy to a senior cat.
With the ever-growing number of pet food options out there, you can rely on these standards to know whether the food that you picked for your pet will have the nutrients they need. If the diet you picked for your pup has the AAFCO label, then you won’t hear many concerns from me.
So, you may be asking yourself, what has Dr. Kritzman fed her dog? Well, Miss Emerald Brown Aria Stark Kritzman has been on everything from Iams to Kirkland to Hills Prescription Renal Diet, and now Purina Bright Minds for Senior Dogs, as she enters her twelfth year. (Not including the countless meals from my children that she’s gotten through counter surfing.)
— Dr. Alyssa Kritzman
Why Tooth Extractions May Be Necessary for Your Pet

When we think about our pets’ health, dental care is often overlooked. However, it plays a critical role in their overall well-being. While the idea of a tooth extraction can sound alarming, it’s sometimes the best and most compassionate option to relieve pain and protect your pet’s health.
Why Would a Tooth Need to Be Extracted?
Veterinarians always aim to preserve teeth whenever possible. However, when a tooth becomes severely damaged or diseased, extraction may be the most effective way to restore comfort and prevent further complications.
Removing a diseased tooth provides several important benefits:
- Eliminates chronic pain that pets often silently endure
- Stops active infections in the mouth
- Prevents harmful bacteria from spreading through the bloodstream to vital organs such as the heart, liver, and kidneys
Left untreated, dental disease can impact far more than just your pet’s mouth; it can affect their entire body.
Common Reasons for Tooth Extractions
There are several conditions that may make extraction necessary:
Severe Periodontal Disease (Bone Loss)
This is one of the most common causes of tooth loss in pets. Periodontal disease occurs when plaque and tartar build up, leading to infection and inflammation of the tissues that support the teeth. Over time, this can destroy the bone holding the tooth in place. When significant bone loss occurs, the tooth becomes unstable and painful, making extraction the best option.
Fractured Teeth with Exposed Pulp
Broken teeth are not just cosmetic issues; they can be extremely painful. When the pulp (the inner part of the tooth containing nerves and blood vessels) is exposed, it leaves the tooth vulnerable to infection. In many cases, extraction is necessary to relieve pain and prevent abscess formation.
Retained Baby Teeth
Sometimes, baby teeth don’t fall out as they should and remain in place alongside adult teeth. These retained teeth can trap food and bacteria, increasing the risk of periodontal disease and misalignment. Removing them early helps maintain proper oral health.
Feline Tooth Resorption
Cats are especially prone to a condition called tooth resorption, where the tooth structure begins to break down from within. This process is painful and progressive, often requiring extraction of the affected teeth to provide relief.
Pets Often Hide Dental Pain
One of the most challenging aspects of dental disease is that pets are very good at hiding pain. Many animals will continue to eat normally even when they have significant oral discomfort. You may not notice any changes in eating habits, which can make dental issues easy to miss.
Subtle signs can include:
- Drooling
- Bad breath
- Pawing at the mouth
- Behavioral changes
However, in many cases, there are no obvious signs at all.This makes regular veterinary exams essential.
How Veterinarians Decide Which Teeth Need Extraction
Determining whether a tooth should be extracted involves a thorough and careful process. During a dental procedure, your veterinarian will:
- Perform a comprehensive oral exam while the pet is under anesthesia
- Use a dental probe to assess gum health and attachment
- Take full-mouth dental X-rays to evaluate the roots and surrounding bone
Dental X-rays are especially important because much of the disease occurs below the gumline, where it cannot be seen with the naked eye. This allows veterinarians to make informed decisions about which teeth can be saved and which are causing pain or infection.
Preventing the Need for Extractions
While some dental issues are unavoidable, many extractions can be prevented with proactive care. Consistent dental care at home is one of the most effective ways to protect your pet’s teeth and gums.
Tooth Brushing Tips
Brushing your pet’s teeth is the gold standard for preventing plaque and tartar buildup. Here’s how to make it easier:
- Start slowly and be patient: Let your pet get used to having their mouth handled before introducing a toothbrush
- Use pet-safe toothpaste: Never use human toothpaste. Pet toothpaste is flavored and safe to swallow
- Choose the right tools: A soft-bristled toothbrush or finger brush designed for pets works best
- Focus on the outer surfaces when first starting: Most plaque accumulates on the outside of the teeth, especially along the gumline. Once your pet is used to having their teeth brushed, you can add in the inner surfaces
- Use gentle, circular motions: You don’t need to scrub hard as gentle brushing is still effective
- Keep sessions short and positive: You can separate your pet’s mouth into four quadrants and reward your pet with their favorite treat after each quadrant is brushed to build a positive association. Aim to brush each quadrant for 30 seconds
- Aim for daily brushing: Consistency matters more than perfection
Additional At-Home Support
- Veterinary-approved dental chews or diets can help reduce plaque
- VOHC approved dental rinses or water additives may also be helpful
- Regularly checking your pet’s mouth for redness, odor, or buildup can help catch problems early
Routine COHATs (Comprehensive Oral Health Assessments and Treatments)
Professional dental cleanings, also known as COHATs, are a cornerstone of your pet’s oral health care. These procedures allow veterinarians to fully assess and treat dental disease in a safe, thorough, and effective way.
A COHAT includes:
- A complete oral examination
- Scaling and polishing of teeth (both above and below the gumline)
- Full-mouth dental X-rays
- Treatment of any identified dental issues
COHATs are best performed under anesthesia. Anesthesia ensures your pet remains still and comfortable, allowing the veterinary team to clean beneath the gumline where the most harmful bacteria reside and to take accurate dental X-rays. Intubation also protects your pet’s airway from water and debris during the procedure.
It’s important to note that anesthesia-free dental cleanings are not recommended. While they may appear less invasive, they only address the visible surfaces of the teeth and do not treat disease below the gumline. Additionally, these procedures typically do not include polishing, which is a critical step after scaling. Without polishing, microscopic defects and rough areas are left on the tooth surface, creating an ideal environment for bacteria to adhere and multiply more quickly. This can accelerate plaque and tartar buildup. Attempting to clean teeth on an awake pet can also lead to stress, incomplete care, and even damage to the teeth or surrounding tissues.
Routine COHATs, combined with at-home dental care, are the most effective way to prevent dental disease and reduce the likelihood of needing extractions in the future.
The Bottom Line
Tooth extractions are never the first choice, but when they are needed, they can dramatically improve your pet’s comfort and quality of life. By addressing dental disease early and maintaining consistent oral care, you can help keep your pet healthy, happy, and pain-free for years to come.
– Dr. Jeanette Barragan
Kitten Season Is Coming
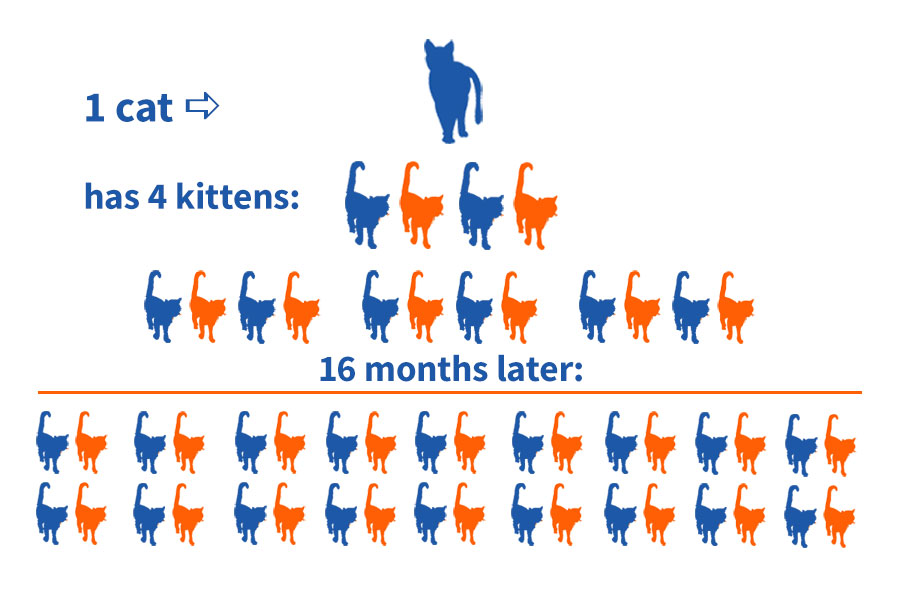
Every spring in Chicago, as soon as the weather shifts, we enter kitten season. And every year, we see the impact of unspayed and unneutered outdoor cats.
If you are feeding outdoor cats in your neighborhood, you are already doing something incredible and compassionate. One important next step to strongly consider is spaying and neutering. It is the single most effective way to prevent suffering and overpopulation.

Cats can become pregnant as early as 4 to 5 months of age and can have multiple litters in one season. One intact female can quickly lead to dozens of kittens. See the chart above to see how quickly one unsprayed cat can multiply! Many of those kittens will face illness, parasites, trauma, and limited access to care.
Spaying prevents life-threatening uterine infections and certain cancers. Neutering reduces fighting, roaming, spraying, and the spread of diseases like FIV. In community cats, Trap Neuter Return programs help stabilize colonies over time. If you notice a tipped ear, that cat has already been sterilized.
If you are caring for outdoor cats and are unsure what your options are, we can help. At Medical District Veterinary Clinic, we are happy to discuss spay and neuter services and connect you with local resources.
Spring is coming. This is the time to plan ahead.
— Ana Valbuena (she/her/ella), DVM
La Temporada de Gatitos Está por Llegar
Cada la primavera en Chicago, en cuanto cambia el clima, entramos en la temporada de gatitos. Y cada año vemos el impacto de los gatos que no están esterilizados y viven al aire libre.
Si estás alimentando gatos en tu vecindario, ya estás haciendo algo increíble y compasivo. Un paso muy importante que debes considerar seriamente es esterilizarlos. Es la manera más efectiva de prevenir el sufrimiento y la sobrepoblación.

Las gatas pueden quedar embarazadas desde los 4 a 5 meses de edad y pueden tener varias camadas en una sola temporada. Una sola hembra sin esterilizar puede resultar rápidamente en decenas de gatitos. Mira la gráfica encima para ver qué tan rápido puede multiplicarse una sola gata sin esterilizar. Muchos de esos gatitos enfrentarán enfermedades, parásitos, traumas y acceso limitado a atención veterinaria.
La esterilización previene infecciones uterinas que ponen en riesgo la vida y ciertos tipos de cáncer. La castración reduce peleas, escapadas, marcaje con orina y la transmisión de enfermedades como el FIV. En gatos comunitarios, los programas de Atrapar, Esterilizar y Regresar ayudan a estabilizar las colonias con el tiempo. Si notas que un gato tiene la punta de la oreja recortada, significa que ya fue esterilizado.
Si estás cuidando gatos afuera y no sabes cuáles son tus opciones, podemos ayudarte. En Medical District Veterinary Clinic estamos disponibles para hablar sobre servicios de esterilización y conectarte con recursos locales.
La primavera ya viene. Es el momento de planear con anticipación.
— Ana Valbuena (she/her/ella), DVM
Let’s Have a Heart to Heart

Introducing Specialty Veterinary Cardiology Services at Our Primary Care Clinic
This month, love is in the air, and we’re celebrating the hearts that matter most—the ones inside your beloved pets. We’re excited to announce that our clinic now offers veterinary cardiology specialty services, including echocardiography (heart ultrasound), provided by a board-certified veterinary cardiologist, right here in the clinic you already know and trust.
What Is a Veterinary Cardiologist?

A veterinary cardiologist is a veterinarian with advanced specialty training focused entirely on heart disease. They partner closely with us as your primary care veterinarians to diagnose, monitor, and manage heart conditions—whether your pet is in the early stages of life or enjoying their golden years.
By bringing cardiology services into our primary care setting, we get the best of both worlds: specialist-level expertise paired with the personalized primary care your pet already receives.
An Echocardiogram: A Big Window into Your Pet’s Heart
An echocardiogram is a noninvasive ultrasound that lets us see the heart in motion—how the chambers fill, how the valves open and close, and how effectively the heart pumps blood.
It’s painless, typically does not require sedation, and provides a lot of information that cannot be obtained from X-rays or physical exams alone. It is one of the best ways for diagnosing most forms of heart disease and determining and evaluating what cardiac medications your pet needs. It also gives us clues on anesthetic safety and whether certain sedatives can be used for procedures.
Echocardiography can help diagnose and monitor many cardiac conditions, including:
- Heart murmurs – A heart murmur is an extra whooshing sound heard when the heart is auscultated. An echocardiogram can sort out innocent murmurs (a harmless sound) from true heart disease
- Degenerative (valvular) heart disease – Common in older, small- and medium-breed dogs
- Dilated cardiomyopathy (DCM) – Often seen in large-breed dogs
- Hypertrophic cardiomyopathy (HCM) – The most common heart disease in cats
- Congenital heart defects – Such as PDA or valve abnormalities
- Arrhythmias (abnormal heart rhythms) – When evaluated alongside ECG findings
- Pericardial disease – Fluid around the heart
- Pulmonary hypertension – Increased pressure in the lungs affecting heart function
Why We Love Offering Cardiology Care
From a primary care veterinarian’s perspective, having a specialist work directly within our clinic is truly special and not something we get the advantage of having every day.
A strong heart team: As your primary care veterinarian, we know your pet. Working hand-in-hand with an on-site cardiologist deepens our knowledge of your pet’s health, helps take guesswork out of complex cardiac cases, and allows for stronger decision making recommendations when it comes to things like anesthesia, surgery, and fluid therapy. That teamwork leads to unified treatment plans, better outcomes and fewer complications.
Less stress, more comfort: Vet visits can be stressful for pets and their owners alike. Receiving specialty care in a familiar environment helps pets (and you) feel more at ease.
Faster answers, better continuity: Because cardiology services are available right here, we can remove the specialty bottleneck and move from concern to diagnosis to treatment without unnecessary delays. And with more data on your pet, we can more specifically target treatment plans to your pet’s needs, sooner, and with more confidence.
Expert care with a personal touch: Our cardiologist collaborates closely with our primary care veterinarians to create treatment plans that are effective, realistic, and aligned with your goals for your pet’s health. The streamlined process means you get personalized answers, faster. We love having cardiology right at our fingertips!
When a Cardio Consult Could Help
Your veterinarian may recommend a cardiology evaluation if your pet has:
- A newly detected heart murmur
- Coughing, exercise intolerance, or breathing changes
- Weakness or fainting episodes
- Known heart disease needing monitoring
- Breed-related risk for heart conditions
- Abnormal findings on X-rays or lab work
- A known heart condition and needs an evaluation before an upcoming anesthetic or surgical procedure
You love your pet, and we do too! And now, advanced heart care doesn’t have to mean leaving the clinic you trust. With specialized veterinary cardiology services and primary care all under one roof, your pet can receive expert cardiac care in a place that already feels like home. Don’t hesitate to ask us if a cardiology consult is right for your pet!
— Amanda Hampton, DVM (she/her/hers)
Importance of Vaccines in Cats and Dogs

As some might have heard, a dog recently tested positive for rabies in Chicago, Illinois. This is the first reported case in Cook County since the 1960s. This development is very alarming and can raise many questions and concerns.
Officials stated that public risk remains low. However, it is very important for pet owners to review current vaccination statuses of ALL pets in the home and monitor for any behavior changes.
Cook County Department of Animal and Rabies Control Confirms Rabies-Positive Dog (cookcountyil.gov)
Vaccines are critical for cats and dogs. They are started at a young age and require a booster dose to ensure adequate immunity. The timing of the booster is also very important. If a shot is missed, then the series must be re-initiated.

There are core vaccines and lifestyle vaccines. Core vaccines are recommended in every patient, whereas lifestyle vaccines are dependent on your pet’s activity and lifestyle.
When you vaccinate your pets, you’re providing them with the immunity needed to fight off potentially life-threatening diseases.
Rabies Vaccine in Dogs AND Cats
Rabies is transmitted via bite wounds, usually by wildlife such as skunks, bats, raccoons, and foxes. This virus attaches to local muscle cells, penetrates local nerves, then ascends to the brain.
There is no reliable, effective treatment for rabies, and infection usually results in death of the infected animal. Once clinical signs are present, death can occur within 10 days. Clinical signs can include restlessness, aggression, excessive drooling, and lethargy.
It is highly recommended to vaccinate at 4 months of age. However, the vaccine can be administered at an earlier age on a case-by-case basis. Early vaccination is common in shelter settings.
The first vaccine is a 1-year vaccine. The following year your pet can get either the 1-year or the 3-year rabies vaccine. Having your pet vaccinated with the rabies vaccine is required by law.
If your pet bites another animal or human and is not up to date on their rabies vaccine, they might have to be confined and observed at a veterinary facility for 10 days. If the animal shows clinical signs or if there is suspicion that the pet might have rabies, their brain tissue must be submitted for sampling. This means that they must be humanely euthanized for tissue submission.
Regulations can vary by state and county, so it is important to keep up with current regulations. You can visit rabiesaware.org for more information regarding regulations in your area.
Prevention consists of vaccination as well as limiting exposure to wildlife.
Please visit your local veterinarian if your pet is not up to date on their rabies vaccine.
Vaccines in Dogs
Distemper (DAPP)
The distemper vaccine protects against the Distemper Virus, Adenovirus 1 & 2, Parvovirus, and Parainfluenza virus. Parvovirus is one of the most common viruses that this vaccine covers.
Without treatment this virus can be fatal. Intensive care (usually is supportive care) is essential for dogs infected with parvovirus. It is important to understand that this can mean a 5- to 7-day hospitalization, potential long-term organ damage, as well as an expensive bill depending on how severe your dog’s signs are. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4951468
The DAPP vaccine is started at 8 weeks of age and must be boostered at least three times, 3 to 4 weeks apart. This means that your puppy will get a DAPP vaccine at 8 weeks old, 12 weeks old, and 16 weeks old. After the initial puppy series, the vaccine becomes annual. A 3-year vaccine is available after the initial series.
Leptospirosis
Leptospirosis is a bacteria that can enter the body via open wounds or mucus membranes. Dogs can become infected via infected urine or infected water and soil. This bacterium can survive for weeks to months in the environment, so it is important to have your pet vaccinated if you live in an area that has a high rodent population.
Leptospirosis is zoonotic which means that humans can get infected as well. Infection can quickly lead to organ damage and can severely affect the liver and kidneys. Clinical signs can be very nonspecific, and treatment consists of antibiotics and supportive care. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4952105
The leptospirosis vaccine is highly recommended in pets living in areas that have a high rodent population, like Chicago. It can be given as early as 12 weeks of age and requires a booster vaccine 3 to 4 weeks after the initial dose. It then becomes annual.
Bordetella
The canine Bordetella vaccine covers Canine Kennel Cough. It is recommended to be given annually or, in some cases, every 6 months.
Bordetella is spread via respiratory secretions from an infected dog. Clinical signs can range from mild to severe symptoms and treatment is dependent on severity. Various boarding and grooming facilities require this vaccine in order to attend their facility. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4951478
Canine Influenza Virus (CIV)
The canine influenza virus vaccine is a lifestyle vaccine recommended in patients that go to frequent boarding or grooming facilities. Clinical signs can be very similar to Bordetella and can include cough, sneezing, and nasal discharge. Outbreaks are most commonly associated with kennels where dogs are in close contact with other dogs. This virus is spread via nasal secretions. The influenza vaccine requires one additional booster given 3 to 4 weeks after the first initial dose; after that it becomes annual.
Lyme
The canine Lyme vaccine is a lifestyle vaccine. It is recommended in dogs that live in highly wooded areas or in pets that frequently go to forest preserves or camping.
Lyme disease is spread via a bite from infected ticks and can be diagnosed with a SNAP 4DX heartworm test, which entails a blood sample for your dog. Clinical signs can vary and can be very nonspecific. Treatment consists of antibiotics and managing secondary symptoms.
Prevention is cheaper than cure. Additionally, ensuring that your dog is on an appropriate flea/tick preventative is important.
The Lyme vaccine can be given any time after 12 to 16 weeks of age and requires one additional booster 3 to 4 weeks after the first initial dose. After that, it is given annually. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4952009
Vaccines in Cats
FVRCP
FVRCP stands for Feline Viral Rhinotracheitis, Calicivirus, and Panleukopenia. These can be very contagious and life-threatening infectious diseases. These viruses can suppress the immune system, leaving the infected individual immunosuppressed and vulnerable to other infectious diseases.
The FVRCP (cat distemper) vaccine series should be started at 6 to 8 weeks of age. This vaccine requires boosters every 3 to 4 weeks until your kitten is 16 weeks old. This vaccine is also available in a 3-year vaccine after your kitten’s initial vaccine series.
Feline Leukemia Virus (FeLV)
The feline leukemia vaccine is highly recommended in indoor/outdoor cats due to their frequent socialization and encounter with other cats. FeLV is spread via close social contact with saliva, blood, urine, or feces. There is no effective treatment. Therefore, treatment consists of supportive care. Prognosis after infection can be variable.
This vaccine series requires a booster 3 to 4 weeks after initial dose.
If your pet is not up to date on their wellness exam or vaccines, please schedule an appointment with your primary care veterinarian.
By Dr. Angélica Calderón
Importancia de las vacunas en gatos y perros
Como algunos habrán oído, un perro en Chicago, Illinois salio positivo recientemente con el virus de la rabia, el primer caso reportado en el condado de Cook desde la década de 1960. Esto es muy alarmante y puede generar muchas preguntas e inquietudes. Las autoridades afirmaron que el riesgo público sigue siendo bajo; sin embargo, es fundamental que los dueños de mascotas revisen el estado de vacunación de todas sus mascotas y estén atentos a cualquier cambio de comportamiento.
Cook County Department of Animal and Rabies Control Confirms Rabies-Positive Dog (cookcountyil.gov)
Las vacunas son fundamentales para perros y gatos. Se inician a una edad temprana y requieren una dosis de refuerzo para asegurar una inmunidad adecuada. El momento de la dosis de refuerzo también es muy importante; si se omite, se debe reiniciar la serie. Existen vacunas esenciales y vacunas adaptadas al estilo de vida. Las vacunas esenciales se recomiendan para todos los pacientes, mientras que las vacunas adaptadas al estilo de vida dependen de la actividad y el estilo de vida de su mascota. Al vacunar a sus mascotas, les proporciona la inmunidad necesaria para combatir enfermedades potencialmente mortales.

Vacuna Contra la Rabia en Perros y Gatos
La rabia se transmite por mordeduras, generalmente de animales silvestres como zorrillos, murciélagos, mapaches y zorros. Este virus se adhiere a las células musculares locales, penetra los nervios locales y luego asciende al cerebro. No existe un tratamiento eficaz y confiable para la rabia, y la infección generalmente causa la muerte del animal infectado. Una vez que aparecen los signos clínicos, la muerte puede ocurrir en un plazo de 10 días. Los signos clínicos pueden incluir inquietud, agresividad, babeo excesivo y letargo.
Se recomienda encarecidamente vacunar a los 4 meses de edad; sin embargo, se puede administrar a una edad más temprana según el caso; esto se hace comúnmente en refugios. La primera vacuna es la del 1 año; sin embargo, al año siguiente, su mascota puede recibir la vacuna antirrábica del 1 año o de los 3 años.
La ley exige que su mascota reciba la vacuna antirrábica.
Si su mascota muerde a otro animal o a una persona y no tiene la vacuna antirrábica al día, podría tener que permanecer confinada y en observación en un centro veterinario durante 10 días. Si el animal muestra signos clínicos o se sospecha que podría tener rabia, se debe enviar su tejido cerebral para su análisis. Esto significa que debe ser sacrificado humanitariamente para el envío de tejido. Las regulaciones pueden variar según el estado y el condado, por lo que es importante mantenerse al día con las regulaciones vigentes. Puede visitar rabiesaware.org para obtener más información sobre las regulaciones en su área. La prevención consiste en la vacunación y en limitar la exposición a la fauna silvestre.
Si su mascota no tiene la vacuna antirrábica al día, visite a su veterinario local. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4951479
Vacunas en Perros
Distemper(DAPP)
La vacuna de distemper protege contra el virus del distemper, adenovirus 1 y 2, parvovirus y virus de la parainfluenza. El parvovirus es uno de los virus más comunes que cubre esta vacuna. Sin tratamiento, este virus puede ser mortal. Los cuidados intensivos son esenciales para el tratamiento de un perro infectado con parvovirus y el tratamiento generalmente es de apoyo. Es importante entender que esto puede significar una hospitalización de 5 a 7 días, así como una factura costosa dependiendo de la gravedad de los síntomas de su perro. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4951468
La vacuna DAPP se inicia a las 8 semanas de edad y debe ser reforzada al menos 3 veces, con 3-4 semanas de diferencia. Esto significa que su cachorro recibirá una vacuna DAPP a las 8, 12 y 16 semanas de edad. Después de la serie inicial para cachorros, la vacuna se vuelve anual, aunque también está disponible una vacuna de 3 años después de la serie inicial.
Leptospirosis
La leptospirosis es una bacteria que puede ingresar al cuerpo a través de heridas abiertas o membranas mucosas. Los perros pueden infectarse a través de orina, agua y tierra infectadas. Esta bacteria puede sobrevivir de semanas a meses en el medio ambiente, por lo que es importante vacunar a su mascota si vive en una zona con una alta población de roedores. La leptospirosis es zoonótica, lo que significa que los humanos también pueden infectarse. Esto puede provocar rápidamente daño orgánico y afectar gravemente el hígado y los riñones. Los signos clínicos pueden ser muy inespecíficos y el tratamiento consiste en antibióticos y cuidados paliativos; sin embargo, en casos graves puede provocar daño orgánico irreversible.
La vacuna contra la leptospirosis es muy recomendable para mascotas que viven en zonas con una alta población de roedores, como Chicago. Puede administrarse a partir de las 12 semanas de edad y requiere una vacuna de refuerzo de 3 a 4 semanas después de la dosis inicial; luego, se vuelve anual.
Bordetella
La vacuna canina contra la Bordetella cubre la tos de las perreras caninas y se recomienda administrarla anualmente; sin embargo, en algunos casos, se recomienda administrarla cada 6 meses. La Bordetella se propaga a través de secreciones respiratorias de un perro infectado. Los signos clínicos pueden variar de leves a graves, y el tratamiento depende de la gravedad. Varias instalaciones de alojamiento y peluquería canina requieren esta vacuna para poder asistir a sus instalaciones. https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4951478
Virus de la influenza canina (CIV)
La vacuna contra el virus de la influenza canina es una vacuna de estilo de vida recomendada para pacientes que asisten frecuentemente a instalaciones de alojamiento o peluquería canina. Los signos clínicos pueden ser muy similares a los de la Bordetella y pueden incluir tos, estornudos y secreción nasal. Los brotes se asocian más comúnmente con perreras donde los perros están en estrecho contacto con otros perros y este virus se propaga a través de secreciones nasales. La vacuna contra la gripe requiere una dosis de refuerzo adicional administrada 3 o 4 semanas después de la primera dosis inicial; después de esa dosis, se vuelve anual.
Lyme
La vacuna canina contra la enfermedad de Lyme es una vacuna que se aplica de su estilo de vida. Se recomienda para perros que viven en zonas boscosas o si su mascota visita con frecuencia reservas forestales o campamentos.
La enfermedad de Lyme se transmite por la picadura de garrapatas infectadas y se puede diagnosticar mediante una prueba de dirofilariosis SNAP 4DX, que requiere una muestra de sangre del perro.
Los signos clínicos pueden variar y ser muy inespecíficos. El tratamiento consiste en antibióticos y el manejo de los síntomas secundarios. Prevenir es más económico que curar, y es importante asegurarse de que su perro reciba un tratamiento preventivo adecuado contra pulgas y garrapatas.
La vacuna de Lyme se puede administrar en cualquier momento después de las 12 a 16 semanas de edad y requiere una dosis de refuerzo adicional de 3 a 4 semanas después de la primera dosis inicial; posteriormente, se administra anualmente.
Vacunas en Gatos
FVRCP
FVRCP significa rinotraqueítis viral felina, calicivirus y panleucopenia. Estas pueden ser enfermedades infecciosas muy contagiosas y potencialmente mortales. Estos virus pueden suprimir el sistema inmunitario, dejando al individuo infectado inmunodeprimido y vulnerable a otras enfermedades infecciosas. La serie de vacunas FVRCP (moquillo felino) debe iniciarse a las 6-8 semanas de edad. Esta vacuna requiere refuerzos y se refuerza cada 3-4 semanas hasta que su gatito tenga 16 semanas de edad. Esta vacuna también está disponible en una de 3 años que se puede administrar el año siguiente después de la serie de vacunas inicial de sus gatitos
Virus de la leucemia felina
La vacuna contra la leucemia felina es muy recomendable en gatos de interior/exterior debido a su frecuente socialización y encuentro con otros gatos. El FeLV (virus de la leucemia felina) se transmite a través del contacto social cercano con saliva, sangre, orina y heces. No existe un tratamiento eficaz, por lo que el tratamiento consiste en cuidados paliativos. El pronóstico tras la infección puede ser variable. Al iniciar esta serie de vacunas, se requiere una dosis de refuerzo 3-4 semanas después de la dosis inicial.
Si su mascota no está al día con su chequeo de bienestar o sus vacunas, programe una cita con su veterinario más cercano.
By Dr. Angélica Calderón
Four Heart Abnormalities Add up to Tetralogy of Fallot

A puppy born with a rare heart condition—Tetralogy of Fallot—got a second chance at life, thanks to a collaboration involving a visiting veterinary heart surgeon and the cardiology and surgery teams at the University of Illinois Veterinary Teaching Hospital.
Odyssey, an Australian shepherd, was only three months old and newly placed in a foster home when he started showing signs of a problem. After exercising, he began breathing heavily and had trouble standing up on his own. He would lean up against the fence just to stay standing and was having uncontrollable tremors. (article continues below)
Cardiology Services at Medical District Vet Clinic
Since November 2025, boarded cardiologists from the University of Illinois Veterinary Teaching Hospital have offered appointments on a part-time basis at the Medical District Veterinary Clinic in Chicago. Services offered include pre-anesthetic echocardiograms, Holter monitoring, management of stable cardiac disease, rechecks, and more. Please call 312-226-2588 to schedule a cardiology appointment for your pet.
Patients with emergent or critical cardiac disease should seek immediate attention and should not wait to see a cardiologist at the clinic.
Dr. Todd Sumerfield, a veterinarian pursuing specialization in veterinary cardiology at the College of Veterinary Medicine, explains how the Illinois team diagnosed Odyssey’s condition and arranged for his surgical intervention—a modified Blalock-Taussig shunt—that had never before been performed at the university hospital.
Diagnosing Tetralogy of Fallot
Noticing Odyssey’s post-exercise behaviors, his foster owners took him to their veterinarian, who identified a loud heart murmur and referred the case to the cardiology team at Illinois in August 2023.
“An echocardiogram was performed, as well as a packed cell volume,” Dr. Sumerfield says.
An echocardiogram allows doctors to visualize the heart as it beats within the patient. In Odyssey’s case, the echocardiogram identified all the defects associated with a condition known as Tetralogy of Fallot.
Packed cell volume measures the amount of red blood cells within the blood of the patient. When an animal has a heart condition leading to decreased oxygen in the blood, as in Tetralogy of Fallot, the body produces more red blood cells in an attempt to deliver more oxygen to the body’s tissues. Although the echocardiographic signs of Odyssey’s condition were severe, his packed cell volume was within the normal range, at 44%.
Dr. Sumerfield points out this normal finding “underlines that Odyssey was doing better than most dogs with this condition at the time of his diagnosis.”
What Is Tetralogy of Fallot?
“Tetralogy of Fallot is an uncommon, congenital heart disease,” Dr. Sumerfield says. “It occurs when the patient has four (thus ‘tetralogy’) concurrent abnormalities.”
To understand these abnormalities, it helps to recall how blood flows through the body. Blood is pumped from the heart’s right atrium to its right ventricle and then, via the pulmonary artery, to the lungs. After receiving oxygen from the lungs, the blood then travels back to the heart into the left atrium. From there it is pumped to the left ventricle, which pushes the blood into the large blood vessel called the aorta and on to the rest of the body.
After delivering its oxygen to tissues and organs, the deoxygenated blood travels back to the right atrium, where the cycle begins again.
In a Tetralogy of Fallot case, the animal is born with a narrowing of the pulmonary valve, which controls blood flow from the right side of the heart to the lungs. The animal also has a ventricular septal defect, which is an inappropriate opening in the septum, or wall, that separates the left and right ventricles. Additionally, the aorta, instead of being positioned over the left ventricle, sits over the left and right ventricular outflow tracts. In that location, the aorta accepts blood from both the left and right ventricles, sending a mixture of oxygenated and deoxygenated blood to the body’s tissues. Lastly, the right ventricle of the heart is abnormally thickened.
Heart Defects Lead to Low Oxygen
Dr. Sumerfield continues, “The narrowing of the pulmonary valve obstructs the outflow of the blood to the lungs. As a consequence, the right ventricle must pump harder to force the same volume of blood through a narrowed orifice.” Because the right ventricle functions just like any other muscle, as it “works out” harder, the muscle grows and thickens.
The ventricular septal defect means deoxygenated blood found in the right ventricle can flow into the left ventricle, where it is pushed into the body without having passed by the lungs to take on oxygen.
All four abnormalities are interrelated and contribute to the problem of low oxygen levels in circulating blood. Abnormally low circulating oxygen led to Odyssey’s exercise intolerance: he was unable to oxygenate his body properly while playing in the yard, making him easily tired.
In response to low oxygen in the body, the bone marrow receives instructions to produce more red blood cells. “When there are inappropriately high numbers of red blood cells in circulation, the blood can become more viscous, or thick. This change, in turn, can impair blood flow to the brain and lead to neurologic signs and even seizures.” Or, in Odyssey’s case, tremors.
Surgery: Modified Blalock-Taussig Shunt
Once Odyssey had a diagnosis, the next step was to determine a treatment approach. It is not typical to treat a patient with Tetralogy of Fallot with medications until there is evidence of heart failure. Phlebotomy (physical reduction of the number of red blood cells) and balloon valvuloplasty (a minimally invasive procedure to widen the pulmonary valve) were considered but both approaches had limitations.
Another option was surgical intervention using the modified Blalock-Taussig shunt. “This surgery involves redirecting mixed arterial blood flow back to the lungs for another pass at oxygenating the red blood cells,” explains Dr. Sumerfield. “The procedure is performed under general anesthesia via a left thoracotomy. A synthetic tube is placed to allow arterial blood to flow to the lungs. The goals of the procedure would be to improve forward flow through the lungs and have a higher percentage of oxygenated blood circulating at any one time.”
A shunt can be thought of as an alternate path, or a turn in the road. It provides the blood with somewhere else to go. Shunts that arise naturally may be present at birth or may be “acquired” by the body after certain stressors. However, in this surgery, an artificial shunt is placed to redirect blood from where it was going into the body (with no oxygen supply) back to the pulmonary artery (which feeds into the lungs) so it can receive its oxygen load.
Odyssey Still Going Strong

Although Odyssey’s clinical signs were not severe, they were getting progressively worse. After his fosters decided to pursue the modified Blalock-Taussig shunt surgery, the University of Illinois cardiology service conferred with surgeons across the country, and Dr. Brian Sutherland, a veterinary cardiothoracic surgeon from the University of Georgia, agreed to perform the surgery. The modified Blalock-Taussig shunt surgery was performed at the Veterinary Teaching Hospital in September 2024, when Odyssey was 1 year, 4 months old. The surgery was successful and Odyssey recovered well.
After two days in the hospital, Odyssey was sent home with pain relievers, sedation, and a strict exercise restriction for two weeks. He was also given six months of blood thinners to decrease the risk of a clot forming in the newly implanted synthetic shunt.
“If left untreated, most dogs with Tetralogy of Fallot will die before reaching one year of age,” says Dr. Sumerfield. “There is limited information regarding life expectancy in dogs who have had the modified Blalock-Taussig shunt procedure, but one journal article found that patients lived for an average of 7 years after the procedure.”
Odyssey is currently more than two years old and continuing to improve. His ability to exercise has improved significantly and his tremors have resolved. Recent rechecks have shown that Odyssey’s shunt is still working.
His fosters have formally adopted Odyssey and are hoping Odyssey lives a long and happy life.
What’s the Deal with Grapes?

Disclaimer: The following is merely surmised from my professional knowledge and opinion on grape toxicity in the field of veterinary medicine, and not my fealty to the Kritzman family creed:
“No raisin shall reside in a baked good where a chocolate chip may be instead.”
The cookie trays and Grandma Sally’s dessert grab bag at the Kritzman family Chanukah party have been a time-honored tradition since before I was born. Now, as a mother myself, I help make the dozen different types of cookies that are needed to provide dessert to the Kritzman clan.
But there is one ingredient I will not bake with in my home, and that’s raisins. We almost never have grapes in the house either. Not because of the Kritzman creed, but because of my dog Emmie. She is our little hoover. As much as I appreciate her cleaning up after my two-year-old’s attempts to make her own taco with shredded cheese, Emmie will not hesitate to eat a grape or raisin if she gets the opportunity.
What’s the big deal about dogs and grape ingestion? Why are they toxic? For much of my career, the veterinary community didn’t really know. We were taught that grapes could be toxic, and even one could put a dog in kidney failure, but we don’t know which dogs or type of grape would cause this.
This lack of knowledge made me loathe grape toxicity as an emergency veterinarian. Not only because of the potential harm it could cause my patients, but it made me feel like a fearmonger to my clients. I had to give people the worst-case scenario for something that might never happen. Although for most dogs the ingestion of one grape won’t cause any problems, for some dogs it could be fatal. And we didn’t know why.
Today, we have more insight. Starting in 2022, tartaric acid (cream of tartar, for us bakers) was seen to cause the same type of kidney damage in dogs as caused by grape toxicity. The problem usually manifests as lethargy, vomiting, diarrhea, and an increase in thirst initially.
Grapes contain tartaric acid, but the concentration of tartaric acid varies wildly between grape varietals and how ripe they are, which makes it quite difficult to calculate an ingested dose. This is why any grape ingestion can be of concern.
So grape toxicity is not a myth or means to rack up the bill at an emergency clinic. If your dog only gets one grape or raisin, you may be in the clear, but you should still reach out to your veterinarian to determine if medical care is needed.
If you’re like me and live with your dog and two semi-feral racoons (a.k.a., small children), you may find it’s just safest to keep grapes and raisins out of the house. Which is not a grave sacrifice for me (see family creed above). I will happily go about baking with chocolate chips, for which I can easily calculate the amount my dog will need to ingest to result in any problems (3 ounces of semi-sweet chocolate). But that is for another blog.
Happy holidays to you all, and best of luck with all the baking!
—Dr. Alyssa Kritzman
Dilated Cardiomyopathy: The Big Heart Disease

This one’s for all the gentle giants, dashing Danes, and persnickety pinschers.
Owners frequently tell others about their dog’s “big heart.” But what if that is not a reference to the dog’s lovable personality? Boarded cardiologists at the University of Illinois College of Veterinary Medicine explain dilated cardiomyopathy, a situation where a “big heart” is not a good thing. (article continues below)
Cardiology Services at Medical District Vet Clinic
Since November 2025, boarded cardiologists from the University of Illinois Veterinary Teaching Hospital have offered appointments on a part-time basis at the Medical District Veterinary Clinic in Chicago. Services offered include pre-anesthetic echocardiograms, Holter monitoring, management of stable cardiac disease, rechecks, and more. Please call 312-226-2588 to schedule a cardiology appointment for your pet.
Patients with emergent or critical cardiac disease should seek immediate attention and should not wait to see a cardiologist at the clinic.
Dilated cardiomyopathy (DCM) affects the muscles of the heart so that they no longer contract forcefully enough to adequately pump blood. This results in an enlargement of the heart, which in turn further impairs the heart’s ability to contract. As this negative cycle continues, the patient becomes increasingly likely to develop congestive heart failure. If congestive heart failure develops, patients will require daily medication and frequent veterinary appointments to monitor their disease.
Who Gets DCM?
Large breed dogs, such as Doberman pinschers, great Danes, and boxers, that are middle-aged or older are predisposed to developing DCM. It may be advisable to screen dogs for the disease if they have a family history of DCM or a predisposition due to their breed.
Factors other than breed may play a role in dogs developing DCM. Over the past few decades, veterinary researchers have published data supporting a link between certain diets and DCM.
These diets are often labeled “grain-free” since they use peas, lentils, other legumes, and potatoes as the main ingredient. It is recommended that dog owners avoid feeding “grain-free” and other diets containing legumes.
What Does DCM Look Like?
DCM is different from other cardiac diseases because it may be present for a long time before the patient shows clinical signs. Even though the patient appears healthy, the disease is present and progressing.
Clinical signs can vary widely between patients with DCM. The first symptoms may be exercise intolerance or lethargy. Patients who have progressed to congestive heart failure can suffer from coughing, collapse, and respiratory distress.
Unfortunately, in some dogs, sudden collapse and even death could be the first sign that anything is wrong. For this reason, screening for DCM and monitoring for progression of the disease are vitally important.
Because DCM affects the heart muscle, it can also cause abnormal heart rhythms, called arrhythmias. Arrhythmias originate in the ventricles, the parts of the heart that pump blood to our lungs and throughout our bodies. In DCM, arrhythmias can occur at the same time or even before changes in the shape and musculature of the heart.
Managing DCM
DCM cannot be cured, but the disease can be managed. The goals of therapy are to improve the heart’s ability to contract, improve clinical signs such as being tired and out of breath, and delay onset of congestive heart failure.
Oral medications are used to improve the efficiency of the heart’s contractions and promote forward flow of blood. Patients with congestive heart failure require additional oral medications to decrease fluid accumulation.
The long-term prognosis for canine DCM can be extremely variable, with some patients rapidly progressing to congestive heart failure and requiring therapy while others remain stable for years. Once congestive heart failure develops, however, patients usually have a poor prognosis. Doberman pinschers also seem to deteriorate more rapidly than other breeds.
Hope for the Future
Having an animal with dilated cardiomyopathy can be scary, but researchers are working on a better treatment. The cardiology service at the University of Illinois participated in a study that evaluates the use of a drug called rapamycin in patients with DCM. Called the REPAIR study, this multi-clinic clinical trial sought to determine if rapamycin will reduce cardiac size and improve contractility in dogs with DCM.
Rapamycin treatment has been shown to reverse age-related declines in cardiac function in both laboratory animals and client-owned dogs, without significant adverse effects.
Maple’s Murmur: A Chihuahua Sees a Heart Specialist

Maple’s owners noticed a problem. Their nine-year-old Chihuahua started to have a dry, hacking cough three to four times a day, mainly in the morning. After coughing for 5 to 10 seconds, Maple would make a retching sound, lick her lips, and then return to normal.
Years earlier, Maple’s primary veterinarian had detected a heart murmur. But because Maple was asymptomatic and the murmur was quiet at that time, they had decided to monitor for changes rather than starting medications or performing other diagnostics. (article continues below)
Cardiology Services at Medical District Vet Clinic
Since November 2025, boarded cardiologists from the University of Illinois Veterinary Teaching Hospital have offered appointments on a part-time basis at the Medical District Veterinary Clinic in Chicago. Services offered include pre-anesthetic echocardiograms, Holter monitoring, management of stable cardiac disease, rechecks, and more. Please call 312-226-2588 to schedule an appointment for your pet.
Patients with emergent or critical cardiac disease should seek immediate attention and should not wait to see a cardiologist at the clinic.
Now the murmur could be heard on both sides of the chest with a stethoscope. Maple had also developed a mild tracheal (windpipe) sensitivity, seen as a soft cough when her veterinarian touched her throat. The rest of her physical exam was within normal limits. Given Maple’s breed, age, and history of progressive heart murmur, her veterinarian suspected she had developed chronic valve disease and suggested that Maple see a veterinary cardiologist.
Dr. Todd Sumerfield, a veterinarian pursuing specialization in cardiology at the University of Illinois College of Veterinary Medicine who cared for Maple, shares the signs and treatments for heart murmurs and chronic valve disease in dogs.
What Are Heart Murmurs?
A heart murmur is a physical exam finding that indicates rapid or turbulent blood flow in the heart or nearby large blood vessels. Murmurs can vary in volume, sound, location, and phase of the cardiac cycle. Even low-grade murmurs can be detected by listening to the heart with a stethoscope.
Murmurs are graded on a scale of 1 to 6, commonly written in Roman numerals (I-VI) in the medical record, with grades given for each side of the chest. Murmurs receive a higher grade as they get louder. A grade V or VI murmur, which can feel like buzzing in a pet’s chest, can even be felt through the skin or heard without a stethoscope.
“While the grade of murmur is helpful to confirm suspicion of heart disease, the grade of murmur does not necessarily correspond with the severity of heart disease,” says Dr. Sumerfield. Additionally, a louder murmur does not always mean worse heart disease than a quiet murmur, and murmur grade cannot be used to monitor disease progression.
Sometimes murmurs are not a sign of disease. These so-called “innocent” heart murmurs are caused by normal blood flow through the heart and are usually harmless.
Pathologic murmurs can be from acquired or congenital disease. Congenital murmurs are present from birth. As in Maple’s case, a veterinarian may hear a heart murmur on physical exam and inform owners that their pet has an underlying heart disease before clinical signs, such as coughing or exercise intolerance, develop. Dr. Sumerfield says small-breed dogs, especially Cavalier King Charles spaniels and toy poodles, have a genetic predisposition to developing chronic valve disease when they are middle-aged or older.
What Is Chronic Valve Disease?
Chronic valve disease (also referred to as degenerative valve disease or myxomatous mitral valve disease) is the most common acquired heart disease in dogs. It typically affects the mitral valve that separates the left atrium and the left ventricle, although other valves may also be affected.
Myxomatous mitral valve disease describes a condition in which a scar-like substance builds up inside the mitral valve, causing it to lose function.
“Myxomatous changes cause the valve to become thickened and irregular, which allows blood to flow backwards across the valve when the heart contracts. This turbulent regurgitation of blood is what causes a heart murmur,” says Dr. Sumerfield.
Maple’s Visit with the Cardiologist
When Dr. Sumerfield examined Maple, he confirmed the presence of a heart murmur and performed an echocardiogram to identify the cause of the murmur. An echocardiogram is a non-invasive ultrasound exam of the heart. It involves shaving small patches of fur on the dog’s chest and may require mild sedation, depending on the temperament of the dog.
Maple’s echocardiogram showed thickened mitral valve leaflets with an enlarged left atrium and ventricle. The mitral valve leaflets are the flaps of tissue that open and close with each heartbeat to control blood flow between the left chambers of the heart.
A technique called color Doppler, which allows for the visualization of blood flow, revealed severe mitral regurgitation as the cause of Maple’s heart murmur.
The echocardiogram confirmed a diagnosis of chronic valve disease in Maple. As this disease progresses, the heart begins to enlarge, which puts the dog at risk of congestive heart failure. That means it is time to intervene medically.
Treatment of Heart Disease
“There are a variety of diseases that cause murmurs, and each is treated differently,” says Dr. Sumerfield. The treatment depends on the underlying cause of the murmur, so proper evaluation is very important. Referral to a veterinary cardiologist may be needed to guide appropriate therapies.
“Most heart diseases may be treated medically. Animals who require medical management will be on oral medications lifelong,” explains Dr. Sumerfield.
Some congenital heart diseases can be cured surgically. Puppies with loud heart murmurs should be evaluated at a young age to determine if they are a candidate for surgery.
In recent years, veterinarians have developed surgical treatment for some forms of acquired heart diseases such as chronic valve disease.
Managing Maple’s Heart Murmur
Maple was sent home on a medication called pimobendan that will help to delay the progression of her heart disease. Before she left, X-rays were taken of her chest so that doctors can monitor the size of her heart and monitor for fluid accumulation in her lungs over time.
Dr. Sumerfield recommends new chest X-rays be performed every six months so her medication can be adjusted to delay congestive heart failure for as long as possible. He also told Maple’s owners that if she experiences difficulty breathing, she would need to see a veterinarian immediately as this may indicate the onset of congestive heart failure. The goal is to keep Maple as happy and healthy for as long as possible without experiencing clinical signs from her heart disease.
This information was originally published on the University of Illinois College of Veterinary Medicine website.
Holiday Pet Hazards: Keeping Your Pets Safe This Season

The holiday season is a time for joy, family, and celebration, but for our pets, it can also be full of hidden dangers. Between festive foods, decorations, and guests coming and going, there are plenty of potential hazards that could put your pets at risk.
Here’s what every pet parent should watch out for to ensure a safe and happy holiday for everyone.
1. Toxic Treats and Dangerous Foods
While it’s tempting to share a little holiday feast with your pet, many traditional foods can be harmful, and in some cases, deadly.
- Chocolate: A classic danger for dogs and cats, especially dark chocolate and baking cocoa.
- Xylitol: Found in sugar-free gum, candies, and some baked goods; it can cause low blood sugar and liver failure in dogs.
- Grapes and Raisins: Common in fruitcakes and cookies, these can cause kidney failure.
- Onions and Garlic: Present in stuffing and gravy, they can damage red blood cells.
- Alcohol: Even small amounts can cause serious health problems.
Tip: Keep food out of reach and remind guests not to feed your pets under the table!
2. Hazardous Holiday Decorations
Decorations add sparkle to your home, but they can be irresistible and risky for curious pets.
- Tinsel and Ribbon: Cats love to bat and chew these, but swallowing them can cause life-threatening intestinal blockages.
- Ornaments: Shiny and tempting, but broken glass or swallowed pieces can injure your pet.
- Christmas Trees: Pine needles can irritate mouths and stomachs; unsecure trees may be tipped over.
- Candles: Keep them out of tail range to prevent burns or fires.
Tip: Opt for pet-safe ornaments and secure your tree to prevent tipping.
3. Plants That Can Poison Pets
Many festive plants are surprisingly toxic to animals.
- Poinsettias: Mildly toxic, causing drooling or stomach upset.
- Mistletoe and Holly: Can cause vomiting, diarrhea, and even cardiovascular issues.
- Lilies: Extremely toxic to cats; even a small nibble can lead to kidney failure.
Tip: Choose pet-friendly silk or artificial plants if you can’t resist the holiday greenery.
4. Cold Weather Concerns
As temperatures drop, our pets face new seasonal risks.

Frostbite and Hypothermia
- Know the signs: Shivering, weakness, and pale or gray skin are warning signs of cold exposure.
- Limit outdoor time: Keep walks shorter during freezing temperatures and avoid prolonged exposure to snow or ice.
- Bundle up: Small breeds, short-haired dogs, and elderly pets may benefit from sweaters or insulated coats.
Cold-Weather Chemicals
Winter brings several products that can be harmful if ingested or absorbed through the paws.
- De-icing salts: Common on sidewalks and driveways, these can cause chemical burns, cracked pads, and stomach upset if licked.
- Ice melt products: Some contain calcium chloride or magnesium chloride, which can irritate skin and paws. Look for pet-safe or “paw-friendly” versions labeled as salt-free.
- Cleaning and snow removal sprays: Certain garage or driveway sprays used for ice prevention may leave harmful residues.
Tips for Protection
- Wipe your pet’s paws and belly with a clean, damp cloth or unscented baby wipes after walks.
- Consider using booties or paw balm to create a protective barrier.
- Designate a pet-safe path or potty area clear of salt and chemical treatments.
Warmth and Comfort Indoors
- Create cozy resting spots: Provide a soft bed away from drafts, cold floors, and space heaters.
- Be cautious with heaters and fireplaces: Pets can burn themselves or knock them over; use guards or barriers for safety.
- Monitor outdoor pets: Bring them indoors whenever possible. If they must stay outside, ensure they have insulated shelter, unfrozen water, and warm bedding.
5. Guests, Noise, and Travel Stress
The hustle and bustle of the holidays can be overwhelming for even the most social pets. Loud music, visitors, and travel can trigger anxiety, especially for pets sensitive to change.
Managing Guests and Parties
- Set boundaries: Create a quiet, pet-only room or area where your pet can retreat during gatherings.
- Keep routines consistent: Feed, walk, and play at your pet’s regular times to reduce stress.
- Watch the doors: With guests coming and going, pets can slip out easily. Consider using baby gates or leashes to prevent escapes.
- Communicate with visitors: Let guests know your house rules such as no feeding table scraps, no letting the cat outside, etc.
Handling Loud Noises and Excitement
- Provide a safe space: Use a crate, cozy corner, or separate room with soft bedding, toys, and background noise (like calm music or a white noise machine).
- Use calming aids: Consider vet-approved pheromone diffusers, anxiety wraps, or natural calming treats. In some cases, anti-anxiety medications may be needed.
Traveling With Pets
- Plan ahead: Make sure your pet is microchipped, has the appropriate vaccinations and has updated ID tags. Always check whether your travel destination or airline requires paperwork for your pet to travel. If so, schedule an appointment within the appropriate time frame and do not wait until the last minute.
- Bring familiar comforts: Pack their favorite blanket, toy, and regular food to ease anxiety.
- Check accommodations: If staying overnight, confirm pet policies and nearby emergency vet locations.
- Secure your pet for car transit: Use a crash-tested carrier or seat belt harness in the car; never let your pet roam freely.
- For long trips: Schedule breaks for water, exercise, and bathroom time.
The best gift you can give your pet this holiday season is safety and peace of mind. By being aware of these common hazards and taking a few preventive steps, you can keep the festivities merry, bright, and pet-friendly.
– Dr. Jeanette Barragan
