Our Blog
Stress and Anxiety in Cats and Dogs

Cats and dogs, just like people, cope with nerves and stress in different ways. For example, Fluffy might tremble his little legs off at his annual wellness exam, while Cleo the cat might need emergency care for a urinary blockage after an owner’s weekend away from home. Coco might attempt to chew the front door down every time mom takes the garbage out, and Simba might react to a new kitten brought home from the shelter by urinating every single place except his litter box.
Pets can display stress and anxiety in various ways, and it is important to recognize the signs, which can impact your pets’ over all well-being. Knowing how to recognize and manage the signs can help your pet feel safe and comfortable in out-of-routine situations or before a known stressor arises.
Owners also need to recognize and distinguish between anxiety and aggression. Fortunately early training and socialization can yield great benefits.
Recognizing Signs
A very common sign of stress is change in overall behavior. Whether a pet is hiding and avoiding interaction or being extremely clingy and constantly seeking attention, any change outside of their usual behavior can be indicative of stress or other potential health concerns. Changes in appetite, both increased and decreased, along with vomiting or diarrhea can also be signs of stress. Any changes to your pet’s behavior requires veterinary input to rule out underlying health conditions as the culprit.
Learn to recognize patterns in your pet’s behavior. For example, if every time there is a thunderstorm, Nala hides in the closet for three days and doesn’t eat any of her favorite treats, maybe we need to pre-treat her with calming supplements or her favorite nature background sounds when it’s raining. If Kitty overgrooms herself every time her pet parents are away for the weekend, maybe she needs anxiety medication while they are away or a daily calming probiotic in the months before the trip.
Pets can’t always tell us when they are stressed or anxious, so they show us. It is important to be able to distinguish those changes. Other signs that can be indicative of stress in a pet include excessive vocalization, destructive behaviors such as excessive chewing/licking or digging, avoidance or hiding, pacing or restlessness, inappropriate urination or defecation, changes in grooming behavior, shaking, panting, drooling, etc.
Common Causes
- Many pets experience separation anxiety when separated from their owners. It is more common in dogs than cats. It is difficult for pets to be left alone for extended periods. Pets with separation anxiety can often display behaviors such as excessive vocalization like barking or howling, destructive behaviors like chewing or biting items or themselves, or showing signs of distress like panting or pacing.
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=10375180 - Situational anxiety is just as it sounds. Pets can get stressed with independent situations such as veterinary visits, car rides, grooming appointments, nail trims, baths, etc. This can also be a trauma response, so a thorough history is important to assess a patient as a whole.
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=10052310
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=10767212 - Dogs and cats have heightened senses and are more sensitive to loud noises. Noise phobia can include thunderstorms, fireworks, and even loud household items, like the blender or the vacuum. Loud knocks from guests or even the garbage truck can cause noise-related anxiety in some pets.
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4952947 - Changes in routine or environment such as moving to a new home, a new person/pet in the home, or just out-of-the-ordinary routine can lead to stress and anxious behaviors. Cats tend to be more sensitive to this than dogs.

Management
There are many ways to help manage stress and anxiety in cats and dogs. However, one shoe does not fit all. What works for one patient may not work for another patient. One patient might need calming music and a pheromone spray prior to a thunderstorm, while another needs a light sedative.
Environmental changes, enrichment, and supplements can serve as great tools to help alleviate mild anxiety and put some patients’ mind at ease in stressful situations. Such tools include calming supplements, pheromone sprays, calming music, calming probiotics, and ThunderShirts®. Helpful environmental changes may include moving Fluffy’s cat tree away from the scary window because he gets startled when the garbage truck passes weekly.
Puzzle toys, snuffle mats, and licking mats are great for enrichment, as they keep patients entertained and their brain stimulated to help cope with stress and anxiety. Licking mats can be a great hit. (Bonus points if you apply peanut butter, canned food, or plain yogurt!) Licking mats can also be frozen to help your pet stay cool in the summertime. Freezing also keeps them busy longer. Make sure you do your research on pet-safe treats.
While supplements and enrichment work well for some patients, others need anxiety medications for stressful situations. Some pets may require daily long-term mediations to manage stress, just as some humans do.
Medical management can sound scary, however there are many medications that can help alleviate stress and anxiety in your pet. Treatment of behavior disorders require training in addition to medications.
- Trazodone is used to manage short -term anxiety, such as vet visits, travel, car rides, thunderstorms, and fireworks. It works by increasing serotonin levels in the brain. Most pets experience relief within just two hours.
- Gabapentin is a multimodal drug that works well for pain, anxiety, and—surprisingly—seizures, depending on the dosing. It is commonly used in cats with situational anxiety and can reach peak activity within two hours.
- Fluoxetine is a long-term daily anxiety medication that is used for humans as well. It is an SSRI (selective serotonin reuptake inhibitor). Serotonin is a neurotransmitter associated with mood. As mentioned, fluoxetine is a long-term anxiety medication, and it may take weeks to see its full effects.
There are many ways to classify anxiety, and many different ways patients show clinical signs of anxiety. If you suspect your pet could be experiencing stress or anxiety, reach out to your local veterinarian or pet behaviorist.
— Dr. Angélica Calderón
Estrés y Ansiedad en Gatos y Perros

Así como las personas les dan nervios y estrés de diferentes maneras, los gatos y los perros también lo hacen. Esto puede variar desde Fluffy temblando con sus pequeñas patitas en su examen anual,o Cleo el gato presentándose en la clínica de emergencias con una obstrucción urinaria después de que su dueño se fue de fin de semana. También por ejemplo, Coco muerde la puerta de entrada cada vez que mamá saca la basura, o Simba orinando en cada planta excepto en su caja de arena después de traer a casa un nuevo gatito de afuera.
Las mascotas pueden mostrar estrés y ansiedad de diferentes maneras y es importante entender y reconocer los signos, causas y formas de manejar estos signos, ya que esto puede afectar el bienestar general de tus mascotas. Saber cómo reconocer y manejar estos signos puede ayudar a que tu mascota se sienta segura y cómoda en situaciones fuera de la rutina o como precaución antes de estresores ya conocidos. También es importante reconocer y distinguir la ansiedad de la agresión y hay grandes beneficios de el entendimiento y socialización temprano.
Reconociendo Señales
Una señal muy común es el cambio en el comportamiento general. Ya sea que una mascota se esté escondiendo y evitando la interacción o sea extremadamente dependiente y busque constantemente atención. Cualquier cambio fuera de su comportamiento habitual puede ser indicativo de estrés u otras posibles preocupaciones de salud. Cambios en el apetito, tanto en aumento como en disminución, junto con vómitos o diarrea, también pueden ser señales de estrés. Sin embargo, es muy importante buscar ayuda veterinaria ante cualquier cambio en tu mascota, ya que otras condiciones subyacentes de salud pueden mostrar señales similares y es importante descartar otras condiciones de salud como la causa.
También es importante reconocer los patrones en el comportamiento de tus mascotas. Por ejemplo, si cada vez que hay una tormenta Nala se esconde en el armario durante tres días y no come ninguno de sus bocadillos favoritos, tal vez debamos darle suplementos calmantes o sonidos de fondo de naturaleza que le gusten cuando llueve. Si Kitty se sobreacicala cada vez que sus dueños están fuera durante el fin de semana, tal vez necesite medicación para la ansiedad mientras están ausentes o un probiótico calmante diariamente meses antes.
Las mascotas no siempre pueden decirnos si están estresadas o ansiosas, así que nos lo muestran y es importante que podamos distinguir esos cambios. Otros signos que pueden ser indicativos de estrés en una mascota incluyen vocalización excesiva, comportamientos destructivos como masticar/lamer o cavar en exceso, evitación o esconderse, andar de un lado a otro o inquietud, micción o defecación inapropiadas, cambios en el comportamiento de acicalamiento, temblor, jadeo, babeo, etc.
Causas Comunes
- La ansiedad por separación es un tipo de estrés que muchos animales experimentan al ser separados de sus dueños, siendo más común en perros que en gatos. Les resulta difícil quedarse solos durante períodos prolongados. Las mascotas con ansiedad por separación pueden mostrar comportamientos como vocalización excesiva, como ladridos o aullidos; comportamientos destructivos, como morder o masticar objetos o a sí mismos; o mostrar signos de angustia, como jadear o caminar de un lado a otro.
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=10375180 - La ansiedad situacional es exactamente lo que suena. Las mascotas pueden estresarse en situaciones independientes como visitas al veterinario, viajes en coche, citas de peluquería, cortes de uñas, baños, etc.
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=10052310
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=10767212 - Los perros y los gatos tienen sentidos agudizados y son más sensibles a los ruidos fuertes. La fobia al ruido puede incluir tormentas eléctricas, fuegos artificiales e incluso elementos ruidosos del hogar como la licuadora o la aspiradora. Cuando los invitados tocan la puerta o incluso el camión de la basura pueden causar ansiedad relacionada con el ruido en algunas mascotas.
https://veterinarypartner.vin.com/default.aspx?pid=19239&id=4952947 - CLos cambios en la rutina o el entorno, como mudarse a un nuevo hogar, la llegada de una nueva persona/mascota en casa, o simplemente salir de la rutina ordinaria, pueden llevar al estrés y comportamientos ansiosos; los gatos tienden a ser más sensibles a esto que los perros.

Mantenimiento
Hay muchas maneras de ayudar a manejar el estrés y la ansiedad en gatos y perros; sin embargo, un enfoque no sirve para todos. Lo que funciona para un paciente no necesariamente significa que funcionará para otro paciente. Un paciente podría necesitar música relajante y un spray de feromonas antes de una tormenta, sin embargo, otro paciente podría necesitar un medicamento sedante ligero.
Los cambios ambientales, el enriquecimiento y los suplementos pueden ser grandes herramientas para ayudar a aliviar la ansiedad leve en algunos pacientes y tranquilizarlos en situaciones estresantes. Estos incluyen suplementos calmantes, sprays de feromonas, música relajante, probióticos calmantes y ThunderShirts®. Esto también puede significar cambios ambientales como mover el árbol para gatos de Fluffy lejos de la ventana aterradora porque se asusta cuando pasa el camión de la basura semanalmente.
Los juguetes rompecabezas y las alfombrillas olfativas son excelentes para el enriquecimiento, ya que mantienen a los pacientes entretenidos y estimulan su cerebro para ayudar a afrontar el estrés y la ansiedad. Los suplementos y el enriquecimiento funcionan muy bien para algunos pacientes, sin embargo, muchos pacientes necesitan medicamentos para la ansiedad en situaciones estresantes y, a veces, incluso mediaciones a largo plazo diarias, al igual que los humanos.
La gestión médica puede sonar aterradora, sin embargo, hay muchos medicamentos que pueden ayudar a aliviar el estrés y la ansiedad en su mascota. El tratamiento de los trastornos de comportamiento requiere entrenamiento además de medicamentos.
- Trazodone es un medicamento que se utiliza para tratar la ansiedad a corto plazo, como visitas al veterinario, viajes, paseos en automóvil, tormentas y fuegos artificiales. Funciona aumentando los niveles de serotonina en el cerebro y la mayoría de las mascotas experimentan alivio en solo dos horas.
- Gabapentin es un fármaco multimodal que funciona bien para el dolor, la ansiedad y, sorprendentemente, para las convulsiones, dependiendo de la dosificación. Esto se usa comúnmente en gatos con ansiedad situacional y puede alcanzar su actividad máxima en dos horas.
- Fluoxetine es un medicamento para la ansiedad de uso diario a largo plazo que también se utiliza para humanos. Es un ISRS (inhibidor selectivo de la recaptación de serotonina), la serotonina es un neurotransmisor asociado con el estado de ánimo. Como se mencionó, la fluoxetina es un medicamento para la ansiedad a largo plazo y puede llevar semanas ver sus efectos completos.
Hay muchas maneras de clasificar la ansiedad y cada paciente que presenta signos clínicos puede ser muy diferente. Hablar con su veterinario es muy importante si sospecha que su mascota podría estar experimentando estrés o ansiedad.
— Dr. Angélica Calderón
It Really Ticks Me Off…

When I started practicing medicine in the dark ages (pre-iPhones) in Chicagoland, the only time I would ever see a tick is after a family came home from a camping trip or a weekend getaway in Wisconsin. Over the past few years, however, ticks have arrived in Chicago.
We have seen several dogs this year with ticks on them, and they haven’t gone farther west than the Kennedy.
Of course, ticks themselves don’t cause the problem: it’s what lurks inside their stomach that can be deadly.
Tick Vomit: Gross and Dangerous
That’s right, tick vomit—or really tick regurgitation into an animal’s bloodstream—is what causes tickborne diseases. A tick attaches to the animal it encounters and embeds its little head into the skin to start their blood meal. When the blood reaches the tick’s stomach, it activates the bacteria that causes the disease. Then the tick regurgitates the bacteria into the animal’s blood.
Depending on the tick and the bacteria, this process can take anywhere from 1 to 2 days. Most preventatives work by killing the tick before it has time to transfer the bacteria into the animal’s bloodstream.

What Does Tickborne Disease Look Like?
There are several different types of bacteria that cause what we call tickborne diseases, but they mostly all belong to the Rickettsial or Borrelia families. The most commonly seen diseases are Lyme, ehrlichiosis, anaplasmosis, and Rocky Mountain spotted fever. There are several other types, though less prevalent in the United States.
These diseases can present in a few different ways. Typically, the pet has fever and lethargy, but these diseases can get into the joints, causing a shifting lameness and puffy joints, a meningitis that can lead to head pressing, or other neurologic signs. They can also cause problems with platelet levels, leading to bruising or more serious issues.
Most of these clinical signs can be resolved with supportive care and the right antibiotic therapy. Unfortunately, dogs can—though rarely—get Lyme nephritis, which can lead to permanent damage of the kidneys and even death.
How Can We Know If Our Animal Was Exposed?
Diagnosis can be a bit tricky. To be honest, experts disagree on the best protocol and test to see if your animal has encountered one of these bacteria.
The most common test that we have in our arsenal is ELISA antibody testing (Idexx 4dx or Antech Accuplex). These tests identify if your dog has antibodies for Ehrlichia, Anaplasma, and Lyme. A positive means that your pet has come into contact with the bacteria, but it doesn’t necessarily mean that have the disease.
A lot of dogs will be able to fight off this disease and will have a positive antibody test, but never become sick. But these bacteria are sneaky little devils. They can lie dormant for months before causing an issue if they don’t cause immediate illness.
It can also take a few weeks if not months for the body to build up an antibody response, so this test may be negative immediately after you find a tick on your pup. We usually recommend getting a baseline test at time of exposure and test again no less than 6 weeks after the tick was found. If we think your dog is sick with a tickborne disease, we may recommend additional tests as well.
When Do We Treat?
This is another topic still being debated in the veterinary community. Some veterinarians believe that any positive test should be treated with antibiotics, while others say only treat when there are clinical signs. Still others say additional testing is needed.
At this time, we recommend treating with antibiotics when there is concern for an active infection, meaning your dog is acting sick. Treatment is usually a course of an antibiotic called Doxycycline.
—Dr. Alyssa Kritzman
Fireworks & Furry Friends: Fourth of July Pet Safety Tips

The Fourth of July is a time for celebration—but for our pets, it can be a source of stress, fear, and potential danger.
At Medical District Veterinary Clinic, we want to make sure your four-legged family members stay safe, calm, and healthy during the holiday festivities. Here are some essential safety tips to help your pet enjoy the holiday as much as you do.
1. Keep Pets Indoors During Fireworks
Even the most confident pets can become terrified by the loud, unpredictable booms of fireworks. To prevent your pet from running away or becoming injured:
- Keep pets indoors well before the fireworks begin.
- Close windows and curtains to reduce noise and flashes of light.
- Play calming music or turn on a TV to help muffle outside sounds.
2. Update Microchip and ID Tags
- Ensure your pet’s microchip is registered and up to date with your current contact information. A microchip greatly increases the chances of being reunited with your pet if they’re found.
- Make sure your pet is wearing a collar with an ID tag that includes your phone number.
3. Create a Safe, Quiet Space
Pets need a place to retreat when they feel overwhelmed. Set up a calm, cozy area in your home where they feel secure:
- Use a crate, a closet, or a quiet room with their favorite toys, bedding, and treats.
- Consider using a white noise machine or fan to drown out external sounds.
- Try a calming pheromone diffuser (like Adaptil for dogs or Feliway for cats).
4. Reduce Stress with Supplements or Medications
Some pets experience severe anxiety during fireworks. Talk to your veterinarian in advance about safe options to ease your pet’s stress:
- Natural calming supplements (such as L-theanine, or calming chews) may help mild anxiety. Some common brand names include Zylkene, Composure, and Solliquin.
- For moderate to severe cases, veterinarian-prescribed anti-anxiety medications can offer effective relief.
- Never give your pet human medications, many of which are toxic to animals.
Plan ahead: Medications often work best when started before the fireworks begin.
5. Outdoor Safety Tips If Your Pet Joins the Celebration
If your pet will be outside during any part of your Independence Day celebration, be mindful of these hazards:
- Keep them far away from fireworks, both used and unused. Fireworks can cause burns, trauma, or poisoning.
- Prevent overheating—make sure pets have access to shade and fresh water, especially during midday heat.
- Secure grills and food—fatty meats, skewers, and aluminum foil can be tempting but dangerous if ingested.
- Watch for citronella candles, sparklers, and glow sticks, all of which can be harmful if chewed or swallowed.
Even social pets can become overwhelmed at parties—always supervise them closely and provide a quiet space to retreat if needed.
Final Thought: Prepare Ahead for a Pet-Friendly Fourth
The Fourth of July doesn’t have to be scary for your pet. With preparation, patience, and a few safety precautions, you can make the holiday fun and stress-free for everyone in your household. If you have any concerns about how your pet may handle the festivities—or need help with medications or supplements—contact us at Medical District Veterinary Clinic today. We’re here to help your pet feel safe, calm, and loved.
Wishing you and your furry friends a happy and safe Fourth of July!
– Dr. Jeanette Barragan
Spay-a-thon 2025: A Win for Pets, Vet Students, and Our Community

On April 26, we hosted our first-ever Spay-a-thon. With the help of our dedicated team and partners, we were able to spay/neuter, vaccinate, microchip, and provide parasite prevention for 79 animals in just one day!
This event would not have been possible without the collective effort of our clinic, our partners at One Tail at a Time and Tree House Humane Society, and Dr. Laura Frazier from the University of Illinois College of Veterinary Medicine community medicine service, who played a key role in planning and execution. By working together, we provided essential care to pets who may not otherwise have had access to these vital services.
Spaying and neutering helps reduce pet overpopulation and keeps animals out of shelters, while vaccinations, parasite prevention, and microchipping ensure these pets stay healthy and safe in their homes. By removing financial and accessibility barriers, we helped pet owners protect their beloved companions while also contributing to a healthier, more responsible pet-owning community.
The Bigger Picture
Events like the Spay-a-thon not only help individual pets but also have a direct impact on public health. By ensuring animals are vaccinated against rabies and other preventable diseases, we help prevent the spread of illness between pets and humans. Parasite prevention further reduces the risks of zoonotic diseases, contributing to a safer, healthier environment for everyone.
As a teaching clinic under the College of Veterinary Medicine, our clinic is always looking for opportunities to provide hands-on educational experiences for veterinary students. This event gave students the chance to gain real-world experience in surgery, anesthesia, and preventive care, all while working alongside experienced veterinarians.
Through mentorship and practical application, students learned not just technical skills, but also the importance of community outreach and accessible veterinary care. Events like these help shape compassionate, well-rounded veterinarians who will carry these lessons into their careers.
Outreach at MDVC
The Outreach Program at the Medical District Veterinary Clinic is committed to building a more diverse and inclusive future for veterinary medicine. Recognizing that the field remains predominantly white, we strive to break down barriers by reaching out to students from underrepresented communities, from elementary school through college.
Our goal is to inspire the next generation of veterinarians by providing mentorship, hands-on learning opportunities, and career guidance. Through interactive workshops, shadowing programs, and community engagement, we aim to foster a deeper connection with the veterinary field, ensuring that the next generation of veterinary professionals reflects the diverse communities they will serve.
Thank You to Our Supporters!
A huge thank you to our veterinary team, students, volunteers, Dr. Laura Frazier, and our incredible partners at One Tail at a Time and Tree House Humane Society for making this event a success. Your dedication and passion are what make events like this possible.
A special thank you to Pete’s Fresh Market #10 (Madison and Western) for donating our water bottles and bananas for our hydration station!
Stay tuned for more details on our Outreach endeavors by keeping an eye on our social media and website for updates! Facebook Instagram
– Ana Valbuena, DVM


Spay-a-thon 2025: Fortaleciendo Nuestra Comunidad, la Salud Pública, y la Próxima Generación de Veterinarios

El 26 de Abril, el equipo de alcance en Chicago de la Clínica Veterinaria Medical District organizó nuestro primer Spay-a-thon. ¡Con la ayuda de nuestro equipo y asociados, pudimos **esterilizar, vacunar, microchip, y brindar prevención de parásitos para 79 animales** en un solo día!
Este evento no hubiese sido posible sin el esfuerzo colectivo de nuestra clínica, nuestros asociados de One Tail at a Time y TreeHouse, y la Dra. Laura Frazier del Programa de Medicina Comunitaria de la Universidad de Illinois, que tuvo un papel clave en la planificación y ejecución. Colaborando, hemos proporcionado cuidados esenciales a mascotas que de otro modo no habrían tenido acceso a estos servicios vitales.
La esterilización ayuda a reducir la superpoblación de mascotas y mantiene a los animales fuera de los refugios, mientras que las vacunaciones, la prevención de parásitos y la colocación de microchips ayudan a que estas mascotas permanezcan sanas y seguras en sus hogares. Al eliminar las barreras económicas y de accesibilidad, ayudamos a los propietarios de mascotas a proteger a sus queridos compañeros, contribuyendo al mismo tiempo a una comunidad de propietarios más sana y responsable.
El panorama más amplio
Eventos como el Spay-a-thon no se limitan a ayudar a las mascotas, sino que afectan directamente a la salud pública. Al garantizar la vacunación de los animales contra la rabia y otras enfermedades prevenibles, ayudamos a evitar la transmisión de enfermedades entre animales de compañía y seres humanos. La prevención de parásitos reduce aún más los riesgos de enfermedades zoonóticas, contribuyendo a un ambiente más seguro y saludable para todos.
Como clínica docente de la Universidad de Illinois, siempre buscamos oportunidades para ofrecer experiencias educativas y prácticas a los estudiantes veterinarios. Este evento brindó a los estudiantes la oportunidad de ganar experiencia en cirugía, anestesia y cuidados preventivos mientras trabajaban junto a veterinarios con mucha experiencia.
A través de la tutoría y la aplicación práctica, los estudiantes aprendieron no sólo habilidades técnicas, sino también la importancia de la ayuda a la comunidad y la atención veterinaria accesible. Eventos como éste ayudan a formar veterinarios compasivos y completos que aplicarán estas lecciones en sus carreras.
Alcance en MDVC
El Programa de Alcance en la Clínica Veterinaria del Distrito Médico se compromete a construir un futuro más diverso e inclusivo para la medicina veterinaria. Reconocemos que el campo sigue siendo predominantemente blanco, por lo que nos esforzamos por romper las barreras y llegar a los estudiantes de las comunidades subrepresentadas, desde la escuela primaria hasta la universidad. Nuestro objetivo es inspirar a la próxima generación de veterinarios, ofreciéndoles tutoría, oportunidades de aprendizaje práctico y orientación profesional. A través de talleres interactivos, programas de observación y la participación de la comunidad, nuestro objetivo es establecer una conexión más profunda con el campo veterinario y lograr que la próxima generación de profesionales veterinarios refleje las diversas comunidades a las que servirán.
¡Gracias a nuestros patrocinadores!
También queremos expresar nuestro sincero agradecimiento a nuestro equipo veterinario, estudiantes, voluntarios, la Dra. Laura Frazier y nuestros increíbles asociados de One Tail at a Time y TreeHouse Humane Society, gracias a los cuales este evento ha sido un éxito. Su dedicación y pasión hacen posible eventos como este.
Queremos expresar un agradecimiento especial a Pete’s Fresh Market \# 10 (en Madison y Western) por donar botellas de agua y bananas para nuestra estación de hidratación.
Para estar al tanto de todo lo relacionado con Outreach, no se pierda nuestras actualizaciones en redes sociales y en nuestro sitio web. Facebook Instagram
– Ana Valbuena, DVM


Meet Dr. Amanda Hampton

Hi everyone! My name is Dr. Amanda Hampton, and I am so excited to be joining the veterinary team at the Medical District Veterinary Clinic.
And I am so excited to meet you! Every person and pet has a different story with different needs. I look forward to getting to know you and finding out how I can best help you and your pet. Until then, here’s a little information for you about me.
My Path to Veterinary Medicine
I grew up in a small, rural community 2 hours west of Chicago, where I loved caring for my family’s personal cats and dogs. In high school, I started working as a paid kennel assistant at my hometown veterinary clinic, cleaning cages, learning about animal husbandry, and observing how the veterinary clinic operated.
That experience was so important and inspired me to pursue a career in veterinary medicine. I was recruited to swim at Western Illinois University, where I earned my undergraduate degree in biology and held part-time positions at a local veterinary clinic and grooming facility.
After undergrad, I was accepted into the University of Illinois College of Veterinary Medicine, where I completed my doctorate. During my time at the college, I loved participating in intramural sports. I eventually met my future husband playing flag football and basketball.
Leading in Practice
After graduation, I started my professional career working at a nationwide corporate preventive care practice where I held roles as a veterinarian, lead doctor, and chief of staff. I loved building the team, creating a culture of safety, and engaging the team to share ideas to improve patient care.
In 2020, the team won the practice’s Chicagoland Veterinary Quality Team of the Year, which was a proud moment in my career.
Eventually, I wanted to further advance and diversify my medical, surgical, and leadership experiences. In 2023, I started a full-time position at a smaller corporate practice. I also started working as a relief veterinarian here at the Medical District clinic and started helping to build their new community outreach program.
Fast forward two years, and now I get to be with them (and you!) full time!
I am so excited to share my passion for the veterinary profession with the clinic and the community. I love being a veterinarian, I love teaching, and I love being able to expose students to this profession.
Access to Veterinary Medicine for All
Accessibility and exposure to the profession are important, and this mindset allows me to honor those who have taught me while giving back to the students who will become the future of veterinary medicine.

A large part of my recent volunteer work included building and co-leading the Diversity, Equity and Inclusion (DEI) committee of the Illinois State Veterinary Medical Association (ISVMA). The committee organizes veterinary student and veterinary professional networking and mentoring events and career fairs for high school students. (Check out the ISVMA “Veterinary Exploration Day” career fair held annually. This year it will be November 8 in Oakbrook, Illinois. Contact ISVMA for more information).
In 2022, the ISVMA DEI committee also helped facilitate transportation for Chicago area students to attend the annual Open House at the University of Illinois College of Veterinary Medicine in Urbana, Illinois. In addition to seeing all the exhibits available to the public, high school students attended a special Q&A with current veterinary students. This event has grown each year and now includes student access to the cultural houses on and tours of the main University campus through the Chicago Village Bus Program.
Ways to Get Involved
These outreach opportunities are an important part in expanding accessibility to care and to the profession. I look forward to seeing how our clinic’s community outreach team can continue to grow these efforts in the Chicago area.
If you are a high school student or guardian, career advisor, and/or community member who knows a student interested in the veterinary profession, please get in contact with us. Opportunities for high school students at our clinic include shadowing a clinician and attending our clinic’s open house for students in June. We also visit high schools to talk about the process of getting into veterinary and veterinary technician school.
Another plug: Vet Med Open House is open to everyone, family friendly, and lots of fun! And it’s free! We hope you get the opportunity to join the event in Urbana, Illinois, on Sunday, October 5.
Outside the Clinic
Outside of the veterinary clinic, I enjoy cooking, being outdoors, practicing yoga, going to Bulls games, and spending time with my family. I live on Chicago’s south side with my husband, who also a veterinarian; our 4-year-old daughter; and a senior Australian shepherd named Brickley.
I look forward to meeting you!
– Amanda Hampton, DVM (she/her/hers)
Urinary Changes in Your Pets

It is always an unhappy surprise when we find a spot of urine somewhere other than the litter box or a potty pad. Especially when it’s on your pile of clothes.
Knowing your pet’s normal urine schedule can be a great help for getting to the bottom of episodes that are outside their routine. Urine changes in a cat or a dog can be caused by very mild to very severe and potentially fatal medical conditions, so it is important to address any changes quickly.
This blog addresses various health conditions that can lead to urinary changes in cats and dogs. You’ll learn clinical signs to watch for, diagnostic tests performed to help determine the cause of these changes, possible medical or surgical treatment options, and what to expect long term.
Urinary Tract Infection (UTI)
The urinary tract consists of the kidneys, the bladder, and the ureters (which carry urine from the kidneys to the bladder). Although a dog or cat can get an infection in any of these three regions, bladder infections are the most common.
Clinical signs may include polyuria, which means frequent urine episodes, such as going in and out of the litter box, or having multiple small streams of urine instead of one large stream. Other clinical signs range from blood in the urine, pain or discomfort when urinating, and posturing to urinate with no urine being produced to odorous urine or lethargy, indicating your pet is not feeling well or is uncomfortable.
An easy inexpensive diagnostic test that can be performed to rule in/out a UTI is a urinalysis. This is a great screening test that allows us to assess the urine for pH changes, specific gravity, crystals, bacteria, white blood cells, etc.
Although a free-catch sample (a sample collected at home) is great, a cystocentesis can be performed in the clinic to obtain a sterile sample. After an ultrasound is used to find the bladder, a sterile needle is inserted to obtain a sample externally. If bacteria are present, the patient has a UTI.
Once a UTI is confirmed, the next step is a urine culture, which means that the laboratory will grow the bacteria in the urine and let us know what antibiotic will treat the infection. Follow-up rechecks with your veterinarian are important to assure that the infection is cleared, as bacteria can become resistant to antibiotics.
Once the infection is gone, the pet’s prognosis is good. Patients with recurrent UTIs may need a long-term prescription urinary diet to keep their pH at a level that does not allow bacteria to grow. This diet will help prevent new infections.
Bladder Stones and Crystals
Stones start off as crystals in the bladder. Crystals may arise due to a variety of factors, such as pH changes and increased urine concentration. Bladder stones come in many types, including struvite, calcium oxalate, urate, cysteine, xanthine, and calcium phosphate.
Fun Facts
- What are the two most common types of bladder stones?
Struvite and Calcium Oxalate - What type of bladder stone is commonly associated with urinary tract infections?
Struvite - Which bladder stone is hormonally dependent and more common in a male dog that has not been neutered?
Cysteine - Why are Dalmatians predisposed to urate stones? (Urate stones are a type of kidney stone formed when uric acid crystals accumulate in the urinary tract.)
Dalmatians have a gene mutation that interferes with uric acid metabolism, causing high levels of uric acid in the body, which concentrates in the urine and leads to stones.
Clinical signs of bladder stones include straining to urinate, dribbling urine, blood in the urine, and pain/discomfort when urinating. Bladder stones can be diagnosed via ultrasound of the bladder and abdominal radiographs. If large enough, they can even be palpated manually. Keep in mind that certain types of bladder stones are not visible on radiographs, so it is important to assess the patient as a whole.
It is always important to check a urine sample to look for an infection. Struvite stones are commonly associated with UTIs. Once the UTI is cleared, then the stone can dissolve.
If a UTI is not present or if a UTI is cleared and a stone remains, then the next step is a prescription urinary diet. The goal of the prescription diet is to change the pH of the urine to allow the stone to dissolve and prevent new stone formation. Some patients may not need to be on a prescription urinary diet long term, however, most patients will.
If the patient is on a urinary diet and the stone is not dissolving or getting smaller, then the next step is surgery. A cystotomy is a surgical procedure performed to remove the stone from the patient’s bladder. Left untreated, stones can become large enough to make urination difficult, which can lead to blockage and life-threatening situations.
Your pet should be urinating daily. A blocked cat or dog is a medical emergency.
Kidney Disease
The kidneys help produce urine and remove toxins from the body. They also help manage hydration, blood pressure, production of red blood cells, and calcium/ phosphorus balance.
The filtration unit of the kidney is called a nephron. As a patient ages, so do the nephrons. If kidney tissue ceases to do its job of filtration, normal function cannot be maintained.
Clinical signs of kidney disease include polyuria (increased frequency of urination), polydipsia (increased water intake), decreased appetite, vomiting, and lethargy in advanced cases.
Kidney disease is diagnosed via blood screening tests along with clinical signs. Kidney disease is irreversible. Treatment depends on the stage and severity of kidney disease. The patent will likely need to be on a prescription kidney diet long term. It is important to check blood pressure, as many patients will have to be on additional medications. If left untreated, kidney disease can be fatal.
Endocrine Conditions
A few conditions related to hormones result in urinary changes in pets.
Hypothyroidism results from decreased thyroid hormone production by the thyroid gland. This condition is more common in dogs than in cats. Clinical signs include weight gain, polyuria, polydipsia, and fatigue.
Hyperthyroidism, on the other hand, is an overproduction of thyroid and is more common in cats. Clinical signs include weight loss, ravenous appetite, polyuria, and polydipsia.
Hypo/hyperthyroidism can be diagnosed via routine blood work and are both medically managed.
Diabetes mellitus is caused by a deficiency in insulin, which is produced by the pancreas. Diabetes can be diagnosed via routine blood work, a fructosamine, along with clinical signs. Clinical signs include polyuria, polydipsia, and weight loss.
With elevated glucose levels in the bloodstream, glucose can spill into the urine in high amounts. Glucose in the urine can lead to bacteria growth leading to urinary tract infections, which are common findings in diabetic patients.
Treatment for diabetes entails daily subcutaneous insulin injections.
Bladder Tumors
Bladder tumors, unfortunately, display similar signs to both urinary tract infections and bladder stones. These include straining to urinate, dribbling urine, blood in the urine, pain/discomfort when urinating, and abdominal pain/discomfort.
A bladder tumor may be suspected if, during a cystocentesis, the ultrasound indicates an abnormality in the bladder. If large enough, bladder tumors can also be seen on radiographs.
Treatment of a bladder tumor depends on the type of tumor and will be determined by working with a veterinary oncologist.
As you can see, urinary changes can range from mild to severe. As veterinarians, our job is to investigate the underlying cause of your pet’s health changes. If you notice any urinary changes in your pet, please see your local veterinarian.
— Dr. Angélica Calderón
Cambios de Orina en Sus Mascotas

Siempre es una gran sorpresa cuando encontramos una mancha de orina de nuestra mascota en algún lugar que no sea apropiado.
Conocer el horario normal de micción de tu mascota puede ser una gran herramienta para lidiar con cualquier episodio que se salga de su rutina habitual. Los cambios en la orina de un gato o un perro pueden ser causados por condiciones médicas desde muy leves hasta muy graves y potencialmente fatales, por eso es importante visitar a su veterinario cuando note cambios de orina en sus mascotas.
Discutiremos varias condiciones de salud que pueden provocar cambios urinarios en gatos y perros y sus signos clínicos a monitorear, pruebas de diagnóstico realizadas para ayudar a determinar la causa de los cambios, opciones médicas o quirúrgicas (si es necesario), mantenimiento y pronóstico.
Infección del Tracto Urinario
El tracto urinario está formado por los riñones, los uréteres y la vejiga. Aunque un perro o un gato pueden contraer una infección en cualquiera de estas tres regiones, las infecciones de la vejiga son las más comunes. Algunos signos clínicos incluyen poliuria (episodios frecuentes de orina), como entrar y salir de la caja de arena o tener múltiples chorros pequeños de orina en lugar de un chorro grande. Otros signos clínicos incluyen sangre en la orina, dolor o malestar al orinar, posturas para orinar sin producir orina, orina con olor y letargo si su mascota no se siente bien o está incómoda.
Una prueba de diagnóstico sencilla y económica que se puede hacer para descartar una infección urinaria es un análisis de orina. Esto nos permite evaluar la orina en busca de cambios de pH, gravedad específica, cristales, bacterias, glóbulos blancos, etc. Aunque una muestra de orina recogida en casa es una buena opción, se puede hacer una cistocentesis en la clínica para obtener una muestra estéril. Esto se realiza mediante el uso de un ultrasonido para encontrar la vejiga; luego se utiliza una aguja estéril para obtener una muestra externa. Si hay bacterias, se confirma la presencia de una infección urinaria en el paciente. Una vez confirmada la infección urinaria, el siguiente paso es un cultivo de orina, lo que significa que el laboratorio hará crecer las bacterias en la orina y nos informará qué antibiótico tratará la infección. Los controles de seguimiento con su veterinario son importantes para asumir que la infección se ha curado, ya que las bacterias pueden volverse resistentes a los antibióticos.
Algunos pacientes con infecciones urinarias recurrentes necesitarán una dieta urinaria prescrita a largo plazo para mantener el pH en un nivel que no permita el crecimiento de bacterias, lo que ayudará a prevenir nuevas infecciones. Una vez que la infección haya desaparecido, el pronóstico es bueno.
Cálculos y Cristales en la Vejiga
Los cálculos comienzan como cristales en la vejiga y pueden deberse a diversos factores, como cambios de pH y aumento de la concentración de orina. Existen muchos tipos de cálculos en la vejiga, como los de estruvita, oxalato de calcio, urato, cisteína, xantina, fosfato de calcio, etc.
Datos curiosos
- Cuáles son los dos tipos más comunes de cálculos en la vejiga?
Estruvita y oxalato de calcio - Qué tipo de cálculo en la vejiga se asocia comúnmente con infecciones del tracto urinario?
Estruvita - Qué cálculo en la vejiga depende de las hormonas y es más común en un perro macho intacto?
Cisteína - Por qué los dálmatas están predispuestos a los cálculos de urato?
Los dálmatas tienen una mutación genética que interfiere con el metabolismo del ácido úrico y causa altos niveles de ácido úrico en el cuerpo, que se concentra en la orina y produce cálculos.
Los signos clínicos incluyen esfuerzo para orinar, goteo de orina, sangre en la orina, dolor o malestar al orinar, etc. Los cálculos en la vejiga se pueden diagnosticar con ultrasonido de la vejiga y radiografías abdominales; si son lo suficientemente grandes, incluso se pueden palpar manualmente si están grandes. Hay ciertos tipos de cálculos en la vejiga que no son visibles en las radiografías, por lo que es importante evaluar a todo el paciente.
Siempre es importante analizar una muestra de orina para evaluar si hay una infección, ya que los cálculos de estruvita se asocian comúnmente con las infecciones urinarias. Una vez que se cura la infección urinaria, el cálculo puede disolverse. Si no hay una infección urinaria o si se cura y queda un cálculo, el siguiente paso es una dieta urinaria recetada. El objetivo de la dieta recetada es cambiar el pH de la orina para permitir que el cálculo se disuelva y evitar la formación de nuevos cálculos. Depende de cada paciente si necesitará seguir una dieta urinaria recetada a largo plazo, pero la mayoría de los pacientes lo harán. Si el paciente sigue una dieta urinaria y el cálculo no se disuelve o no se hace más pequeño, el siguiente paso es la cirugía. Una cistotomía es un procedimiento quirúrgico que se realiza para extraer el cálculo de la vejiga del paciente. Si no se trata, los cálculos pueden llegar a ser lo suficientemente grandes como para dificultar la micción, lo que puede provocar un bloqueo y situaciones potencialmente mortales. Su mascota debe orinar a diario. Un gato o perro bloqueado es una emergencia médica.
Enfermedad Renal
Los riñones ayudan a producir orina y a eliminar toxinas del cuerpo. También ayudan a controlar la hidratación, la presión arterial, la producción de glóbulos rojos y el equilibrio calcio/fósforo. La unidad de filtración del riñón se llama nefrona. Cuando una mascota envejece, las nefronas también envejecen. Sin tejido renal funcional no se puede mantener una función normal. Los signos clínicos de la enfermedad renal incluyen poliuria (aumento de la frecuencia de micción), polidipsia (aumento de la ingesta de agua), disminución del apetito, vómitos y letargo si está avanzado.
La enfermedad renal se diagnostica por análisis de sangre y signos clínicos. La enfermedad renal es irreversible y el tratamiento depende de la etapa de la enfermedad y de lo avanzada que esté. Es probable que el paciente deba seguir una dieta renal recetada a largo plazo. Es importante controlar la presión arterial, ya que muchos pacientes deberán tomar medicamentos adicionales. Si no se trata, la enfermedad renal puede ser mortal.
Condiciones de Endocrinas
El hipotiroidismo es el resultado de una disminución de la producción de hormona tiroidea por parte de la glándula tiroides, más común en los perros. Los signos clínicos incluyen aumento de peso, poliuria, polidipsia y fatiga. Por el contrario, el hipertiroidismo es más común en los gatos y es la sobreproducción de hormonas. Los signos clínicos incluyen pérdida de peso, apetito voraz, poliuria y polidipsia. El hipotiroidismo y el hipertiroidismo se pueden diagnosticar mediante análisis de sangre de rutina y ambos se tratan con medicamentos. Como puede ver, estas afecciones también implican cambios urinarios en una mascota.
La diabetes mellitus es causada por una deficiencia de insulina, que es producida por el páncreas. La diabetes se puede diagnosticar mediante análisis de sangre de rutina, una fructosamina, junto con los signos clínicos. Últimamente, el tratamiento implica inyecciones subcutáneas diarias de insulina. Los signos clínicos incluyen poliuria (micción excesiva), polidipsia (ingesta excesiva de agua) y pérdida de peso. Con niveles elevados de glucosa en el orine, la glucosa puede derramarse en la orina en grandes cantidades. La glucosa en la orina puede provocar el crecimiento de bacterias que provocan infecciones del tracto urinario, que son hallazgos comunes en pacientes diabéticos.
Tumores de Vejiga
Los tumores de vejiga pueden presentar síntomas similares a las infecciones del tracto urinario y a los cálculos vesicales, como esfuerzo para orinar, goteo de orina, sangre en la orina, dolor o malestar al orinar y dolor o malestar abdominal. Se puede sospechar un tumor de vejiga si se observa una anomalía en ultrasonido mientras se examina la vejiga durante una cistocentesis. Si son lo suficientemente grandes, los tumores de vejiga también se pueden ver en las radiografías. Una vez que se diagnostica un tumor de vejiga, el tratamiento se basa en el tipo de tumor. Aquí es donde el dueño de la mascota trabajará junto con un oncólogo veterinario para determinar el mejor plan de tratamiento para su mascota.
Como puede ver, los cambios urinarios pueden variar de leves a graves y nuestro trabajo como veterinario es investigar la causa subyacente de los cambios en la salud de su mascota. Si nota algún cambio urinario en su mascota, consulte a su veterinario local.
— Dr. Angélica Calderón
Meet Your Microbes

A few months ago, I had the opportunity to represent our clinic at a conference entitled Combating Antimicrobial Resistance with Stewardship, hosted by the Chicago Department of Public Health. It was wonderful to see professionals in all different sorts of medical fields come together to discuss topics that affect us all in how we manage our ever-developing love-hate relationship with these bugs that live all around and inside of us.
The average person has 38 trillion bacterial cells inside of them. These microbes are just as much of us and our pets as our very own cells. Bacteria are vital to our daily lives and the lives of our pets. Our understanding of our relationship with these little guys is constantly evolving. That’s why I feel it’s important to review some of the terminology related to the medications and practices used to manage bacteria.
Microbiome
This is a catchall word that refers to all the single-cell organisms that live in the body. The microbiome includes all bacteria, viruses, fungi, and protozoa that can be found inside and on the body of any animal. There are good bugs and bad bugs. They can affect everything from the smell of our breath to rashes on our skin.
People often think “microbiome” relates just to the digestive system, but it also includes any organ system where these little ones can live, such as the skin, reproductive systems, oral cavity, and respiratory systems. For the most part, these organisms live in harmony with the animal’s body. When there is an imbalance, however, or some of these critters take up space where they don’t belong, the result can mean illness for us and our pets.
Probiotics
A probiotic is a bacterium that has been found to improve gut health. (You may see probiotic products for people for other parts of the body, but in veterinary medicine probiotics almost exclusively relate to the GI system.)
For our dogs and cats especially, gut health is determined by stool quality. Diarrhea in a pet is often a sign that pathologic (bad) bacteria and other microorganisms have overpopulated. In these cases, introducing a good bacteria can help reestablish balanced populations of bacteria and improve stool quality.
Many veterinary studies in recent years have shown that giving a probiotic helps control diarrhea faster than giving an antibiotic. Plus, probiotics may make diarrhea less likely to return in the future.
Antibiotics
These don’t need a lot of explanation, but just so that we’re all on the same page, antibiotics are medications that kill bacteria by targeting cellular function that is specific to bacterial cells and not our cells.
There are different kinds of antibiotics, categorized by what kinds of bacteria they attack, how powerful they are, and how they work (e.g., by killing the bacteria or just keeping them from reproducing).
The discovery of antibiotics is arguably the most important discovery of modern medicine. But it is also important to note that the more we use these drugs the less effective they can get. It’s vital that veterinarians and other medical professionals be judicious with their use.
Antiseptics
These are compounds that try to kill any microbial life. They don’t have to be specific to one type of bacteria or virus. These are most often used topically on the skin or cleaning surfaces. I feel that we often skip over antiseptics and think only of antibiotics, but antiseptics can be a valuable tool in keeping our pets healthy and keeping the bad bacteria under control
Prebiotics
This term is a bit newer to many of us. For a long time, most medical professionals thought you could manage the microbiome either by trying to take away bad bugs (using antibiotics and such) or by adding probiotics. Recently, attention has turned to prebiotics, especially among dog food companies.
Prebiotics are typically non-soluble (meaning we don’t absorb them) foods that the “good” bugs in the microbiome like. It may seem a bit obvious, but it’s a lot easier to put food into dog and cat food than to put probiotics into a food. A probiotic has to be alive to perform its function, but food is food. Prebiotics give the good bacteria the fuel they need to thrive, which is easier to do than delivering living good bacteria.
So, there’s your refresher! I hope it was a lot less painless than all of the microbiology classes I had to take in veterinary school. I still shudder thinking about trying to remember which viruses have cellular membranes or whether or not certain protozoa are found in certain chambers of a cow’s stomach.
Now go have a banana-oat-kefir milk smoothie and give those little buggers a treat!
Alyssa Kritzman, DVM
Feature illustration from AdobeStock images
Maintaining Your Pet’s Dental Health

As pet owners, we all want to ensure our furry companions live long, healthy, and happy lives. One of the most important aspects of your pet’s overall health is their dental care, yet it often goes unnoticed.
Did you know that by the time most pets are just a few years old, they may already be suffering from some form of periodontal disease? This blog will explore the significance of dental health in pets, discuss the common signs and stages of periodontal disease, and offer tips on how you can help keep your pet’s teeth and gums healthy at home.
What Is Periodontal Disease?
Periodontal disease is a progressive condition that affects the tissues surrounding the teeth, including the gums, bone, and ligaments. It begins with the accumulation of plaque and tartar on your pet’s teeth, which harbor bacteria that cause inflammation and infection in the gums. If left untreated, periodontal disease can lead to tooth loss, chronic pain, and systemic infections that can affect your pet’s overall health.
There are four stages of periodontal disease:
Stage 1 – Gingivitis: In this early stage, your pet’s gums become inflamed and red. There is no permanent damage to the teeth or surrounding tissues, but if untreated, it can progress to more severe forms of the disease.
Stage 2 – Early Periodontitis: At this stage, plaque and tartar have begun to accumulate below the gumline. Gums may recede slightly, and some bone loss may occur, but the damage is still minimal.
Stage 3 – Moderate Periodontitis: This stage is characterized by significant gum recession, further bone loss, and infection. Pets may show signs of discomfort, and tooth mobility can start to become noticeable.
Stage 4 – Advanced Periodontitis: This is the most severe stage, where there is extensive gum recession, significant bone loss, and tooth instability. Pets at this stage may experience severe pain and infection that can spread throughout their body.
Common Symptoms of Periodontal Disease
Periodontal disease often develops slowly, and many pets don’t show obvious symptoms until the condition is advanced. However, there are several warning signs to watch for:
- Bad breath (halitosis)
- Red or swollen gums
- Drooling or excessive salivation
- Difficulty chewing or reluctance to eat hard food
- Loose or missing teeth
- Pawing at the mouth or face
- Changes in behavior, such as irritability or reluctance to be handled around the mouth
One critical thing to note is that many pets, especially dogs and cats, will continue eating even with significant dental pain. This makes it even more important to be proactive about your pet’s dental care since the discomfort may not always be immediately obvious.
When Does Periodontal Disease Develop in Pets?
Studies show that periodontal disease can start as early as three years of age in cats and dogs. In fact, around 80% of dogs will have some form of periodontal disease by the time they reach three years old. For cats, around 70% show signs of dental disease by the age of three.
While these numbers may seem alarming, the good news is that periodontal disease is largely preventable with regular dental care.
The Importance of Dental Health
Maintaining your pet’s dental health is about more than just preventing bad breath and tooth loss. Untreated periodontal disease can lead to significant pain, and the bacteria from infected gums can enter the bloodstream and affect vital organs like the heart, kidneys, and liver. This can lead to systemic health issues that can shorten your pet’s lifespan.
Regular dental care can prevent these complications and keep your pet pain-free, allowing them to live a longer, healthier life. Early detection and treatment of periodontal disease are key to avoiding severe complications and ensuring your pet’s comfort and well-being.
Tips for Regular Dental Care at Home
The good news is that with a little effort, you can help your pet maintain optimal dental health at home. Here are some effective ways to manage your pet’s dental hygiene:
- Brushing Your Pet’s Teeth: Brushing your pet’s teeth is one of the most effective ways to prevent plaque and tartar buildup. Aim to brush your pet’s teeth daily using a pet-safe toothbrush and toothpaste. Start slowly, allowing your pet to get used to the process, and always use products designed for pets. (Human toothpaste contains ingredients that can be harmful to animals.)
- Water Additives: Dental water additives can be a simple solution to help reduce plaque and tartar. These additives are mixed with your pet’s drinking water and can help maintain oral hygiene with minimal effort.
- Dental Chews and Treats: Many commercial dental chews are designed to help reduce plaque and tartar through chewing action. Look for products that are approved by the Veterinary Oral Health Council (VOHC) for proven effectiveness.
- Dental Toys: There are a variety of dental toys available that help massage your pet’s gums and scrape plaque off their teeth while they play. Always ensure any toy or treat can be indented with your fingernail to ensure that it is safe enough for your pet’s teeth and won’t cause fracture of any teeth.
- Healthy Diet: Providing your pet with a balanced diet can contribute to their overall health, including their oral health. Some specially formulated dental diets can help control plaque and tartar buildup.
Professional Dental Cleanings
Even with the best at-home care, your pet will still need professional dental cleanings from time to time. Veterinarians use specialized equipment to thoroughly clean the teeth and gums, removing plaque and tartar that may be hard to reach with regular brushing. Professional cleanings are usually done under anesthesia to ensure that your pet remains still and comfortable throughout the procedure.
Dental cleanings not only help treat existing periodontal disease, but they also give your veterinarian the opportunity to spot potential issues before they become more serious. For pets with significant dental disease, extractions may be necessary to prevent further pain or infection.
Conclusion
Dental health is an integral part of your pet’s overall well-being. Periodontal disease is common, but it is also preventable with regular dental care. By brushing your pet’s teeth, using water additives and dental chews, and scheduling routine professional cleanings, you can help keep your pet’s teeth and gums healthy, prevent systemic disease, and improve their quality of life. So, take charge of your pet’s dental health today, and enjoy the peace of mind that comes with knowing you’re doing everything you can to keep them happy and healthy for years to come.
– Dr. Jeanette Barragan
Cold Weather Cautions for Your Pets

With cooler temperatures approaching, it is important to take precautions to keep your pets safe and warm throughout the winter months.
Prolonged exposure to extreme cool temperatures can lead to frostbite, causing tissue damage to exposed areas, and hypothermia, a life-threatening drop in body temperature. Senior pets, along with very young pets or those with chronic illnesses, are more vulnerable. This becomes important for dogs and cats with arthritis, as cooler temperatures can lead to stiff joints and increased pain in the winter months.
At temperatures above 45°F most dogs are comfortable and safe outside for regular activities like walks and playtime. However, temperatures 45°F or below can cause discomfort in small, thin-coated, senior, immunocompromised, or ill dogs.
Frostbite and hypothermia become risks at temperatures below 32°F, especially in breeds not adapted to cold climates. At temperatures below 0°F, dogs should be allowed outside only for short bathroom breaks. Even hardy breeds can suffer frostbite and hypothermia quickly in these temperatures.
Cats are more vulnerable as temperatures drop below 32°F. Cats should remain indoors as much as possible, as even short exposure can cause frostbite or hypothermia. Frostbite risk areas include ears, tails, and paws. These areas are most susceptible to frostbite because they have less fur and are prone to freezing.
Symptoms of hypothermia include shivering, lifting paws off the ground, whining or attempting to return indoors, lethargy, stiff muscles, slow breathing, and pale or blue gums. This can be life-threatening!
Precautions for Your Dogs
Know your dog’s cold tolerance and limit time outside. Try to keep your dog indoors as much as possible while ensuring that they get enough exercise. Shorten walks in extremely cold weather and keep your dog active indoors by providing enrichment and indoor play.
Avoid shaving your dog’s coat during winter as their natural fur provides insulation. Regular brushing can also help their coat retain warmth. Dry your dog thoroughly after exposure to rain or snow to prevent them from getting cold.
Use warm, durable winter coats and jackets, especially for short-haired or small breed dogs. Booties and paw wax protects paws from ice, snow, and harmful chemicals like salt. Consider protective paw balm to help prevent cracking and irritation from cold surfaces and ice melt. Rock salt and other chemicals used to melt snow and ice can irritate your pet’s paw pads and, if licked off the paws, their mouth. Be sure to wipe all paws with a damp towel before your pet licks them. Dogs are at particular risk of salt poisoning during the winter due to the rock salt used, often from licking their paws after a walk. There are many pet-safe ice melt options available.
Antifreeze has a sweet taste that may attract animals. Choose a pet-safe antifreeze because even small amounts of antifreeze can be lethal. Clean any antifreeze spills immediately and keep it out of reach. Coolants and antifreeze made with propylene glycol are less toxic to pets.
What About Outdoor Cats?
Outdoor cats need extra care as they often roam unsupervised. If possible, bring cats indoors during extreme weather. Subzero temperatures, snowstorms, or icy conditions are too dangerous for outdoor cats, so they should be temporarily housed indoors. If housing indoors is not possible, then providing outdoor shelter is very important. Create a weatherproof, insulated shelter with an entrance just large enough for a cat. Line the shelter with straw, as straw repels moisture and provides better insulation than blankets. Cats often seek warmth under car hoods so be very cautious when starting your car in the morning.
In freezing weather, outdoor cats might struggle to find unfrozen water or sufficient prey, leading to dehydration and malnutrition. There are many ways we can help keep outdoor cats safe this winter. Outdoor cats require extra calories to maintain body heat, so proper nutrition is important. Using heated water bowls and replacing water frequently is important to prevent freezing water. Avoid metal bowls as tongues can stick to frozen surfaces.
By taking these precautions, you and your pet can stay warm and healthy this winter.
By Dr. Angélica Calderón
Precauciones Para Sus Mascotas en Climas Fríos
Con la llegada de las temperaturas frías, es importante tomar todas las precauciones adecuadas para mantener a sus mascotas seguras y abrigadas durante los meses de invierno.
La exposición prolongada a temperaturas extremadamente frías puede provocar congelación, e hipotermia, una caída de la temperatura corporal potencialmente mortal. Las mascotas mayores y las muy jóvenes o aquellas con enfermedades crónicas son más vulnerables. Esto es importante para los perros y gatos con artritis, ya que las temperaturas frías pueden provocar rigidez en las articulaciones y aumento del dolor en los huesos.

A temperaturas superiores a 45 °F, la mayoría de los perros se sienten cómodos y seguros afuera para actividades como paseos y juegos. Sin embargo, las temperaturas de 45 °F o menos pueden causar molestias en perros pequeños, de pelaje fino, mayores, inmunocomprometidos o enfermos. La congelación y la hipotermia se convierten en riesgos a temperaturas inferiores a 32 °F, especialmente en razas no adaptadas a climas fríos. Los gatos son más vulnerables cuando las temperaturas caen por debajo de los 32°F. A temperaturas inferiores a 0 °F, deje que los perros salgan solo para breves descansos para ir al baño. Incluso las razas vulnerables pueden sufrir congelación e hipotermia rápidamente con estas temperaturas. Los gatos deben permanecer en el interior el mayor tiempo posible, ya que incluso una exposición breve puede provocar congelación o hipotermia. Las áreas de riesgo de congelación incluyen orejas, colas y patas. Estas áreas son más susceptibles a la congelación porque tienen menos pelaje y son propensas a congelarse.
Los síntomas de hipotermia incluyen escalofríos, levantar las patas del suelo, gemir o intentar regresar al interior, letargo, rigidez muscular, respiración lenta y encías pálidas o azules. ¡Estos pueden poner en peligro la vida!
Precauciones Para los Perros
Conozca la tolerancia al frío de su perro y limite el tiempo que pasa afuera. Trate de mantener a su perro adentro el mayor tiempo posible, pero asegúrese de que aún haga suficiente ejercicio. Acorte las caminatas en climas extremadamente fríos y mantenga a su perro activo en el interior brindándole enriquecimiento y juego en el interior.
Evite cortar el pelo de su perro muy corto durante el invierno, ya que su pelaje natural le proporciona aislamiento. El cepillado regular también puede ayudar a que su pelaje retenga el calor. Seque bien a su perro después de exponerlo a la lluvia o la nieve para evitar que se enfríe.
Utilice abrigos y chaquetas de invierno cálidos y duraderos, especialmente para perros de pelo corto o de razas pequeñas. Los botines y la cera para patas protegen las patas del hielo, la nieve y productos químicos como la sal. Considere utilizar un bálsamo protector para las patas para ayudar a prevenir la irritación causadas por las superficies frías y el hielo derretido. La sal de roca y otros productos químicos utilizados para derretir la nieve y el hielo pueden irritar las almohadillas de las patas de su mascota. Asegúrese de limpiar todas las patas con una toalla húmeda antes de que su mascota las lama e irrite su boca. Los perros corren un riesgo particular de intoxicación por sal durante el invierno debido a la sal de roca utilizada, casi siempre por lamerse las patas después de un paseo. Hay muchas opciones disponibles para derretir hielo apto para mascotas.
El anticongelante tiene un sabor dulce que puede atraer a los animales. Elija un anticongelante apto para mascotas, ya que el envenenamiento por anticongelante puede ser letal incluso en pequeñas cantidades. Limpie cualquier derrame de anticongelante inmediatamente y manténgalo fuera de su alcance. Los refrigerantes y anticongelantes elaborados con propilenglicol son menos tóxicos para las mascotas.
Y Los Gatos de Afuera?
Los gatos que viven afuera necesitan cuidados especiales, ya que andan sin supervisión. Si es posible, lleve a los gatos al interior durante condiciones climáticas extremas. Las temperaturas bajo cero, las tormentas de nieve o las condiciones heladas son demasiado peligrosas para los gatos que viven afuera y deben de mantenerlos temporalmente adentro. Si no es posible, es muy importante proporcionar refugio afuera. Cree un refugio aislado y resistente a la intemperie con una entrada lo suficientemente grande para un gato. Cubra el refugio con paja, ya que la paja repele la humedad y proporciona un mejor aislamiento que las cobijas. Los gatos suelen buscar calor debajo del capó de los coches, así que hay que tener mucho cuidado.
En climas helados, los gatos de afuera pueden tener dificultades para encontrar agua no congelada o presas suficientes, lo que provoca deshidratación y desnutrición. Hay muchas maneras en que podemos ayudar a mantener seguros a los gatos de afuera.
Los gatos de afuera necesitan calorías adicionales para mantener el calor corporal, por lo que una nutrición adecuada es importante. Es importante utilizar calentadores de agua y reemplazar el agua con frecuencia para evitar que se congele. Evite los tazones de metal ya que la lengua puede pegarse a las superficies congeladas.
Si toma estas precauciones, usted y su mascota podrán mantenerse abrigados y saludables este invierno.
By Dr. Angélica Calderón
Take a Peek at My ‘Other’ Workplace

As many of you know, but others may not, in January I stepped into the role of interim director of the University of Illinois Veterinary Teaching Hospital in Urbana, while continuing to serve as medical director of Medical District Veterinary Clinic here in Chicago.
Unfortunately, a nationwide search for a permanent director of the teaching hospital did not result in a successful hire. The dean of the veterinary college has asked me to stay in my interim role through 2026, and I have agreed. While I am honored to help and enjoy the work in Urbana, I also miss seeing many of you and your pets.
Over the next two years I will remain actively involved in the daily operations of the Medical District clinic. I plan to continue seeing patients one day a week in Chicago. We are in the process of hiring another veterinarian for the Chicago clinic to help manage caseload and provide more availability for your pets.
In this blog, I want to tell you a little about the teaching hospital and showcase some exciting developments there.
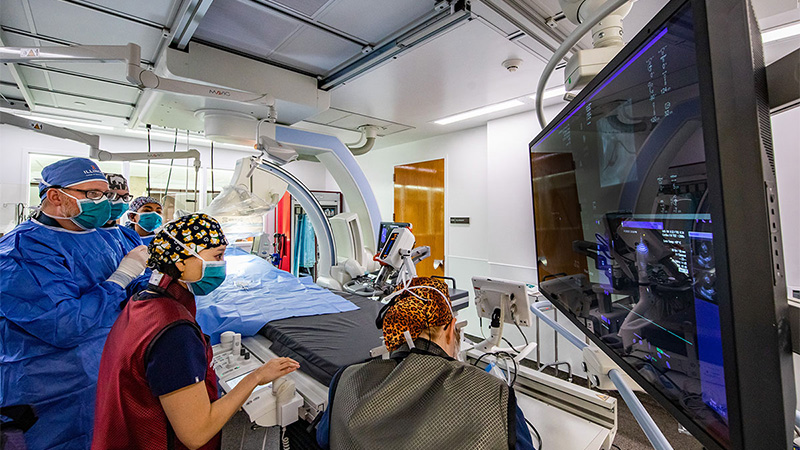

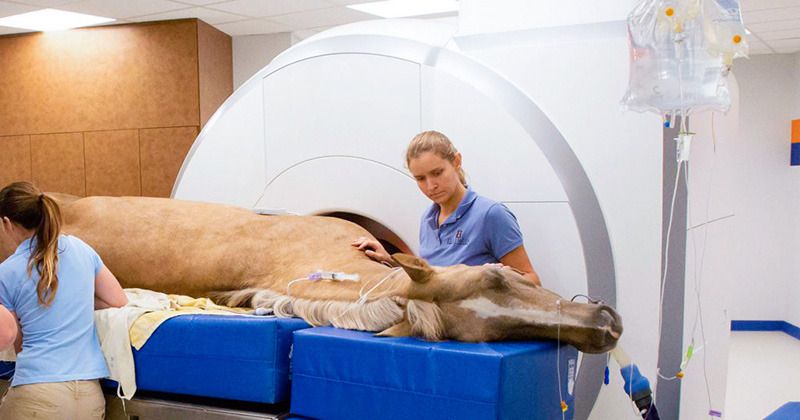



The Veterinary Teaching Hospital is a leading multi-specialty referral and emergency center, recognized nationally for its research, clinical care, and veterinary education. Organizationally within the College of Veterinary Medicine, the Medical District Veterinary Clinic is actually a satellite facility of the teaching hospital.
As interim director, I have the privilege of working alongside an exceptionally talented team of over 70 clinical faculty members and 180 support staff, across a wide range of specialties, from anesthesiology/pain management to cardiology, neurology, ophthalmology, and zoological medicine. In addition to the Medical District clinic, our facilities include the Small Animal Clinic, Large Animal Clinic, Midwest Equine, and Vet Med South Clinic.
Many features you’d expect in a human medical center can be found there:
- A linear accelerator for advanced radiation therapy
- A 3-Tesla MRI and CT scanner for high-resolution imaging
- Eight small animal surgery suites, including an interventional suite for procedures such as surgical repair of heart defects
- Advanced imaging and surgical capabilities for equine and food animal patients.
We also provide 24-hour emergency services for all domestic species, a wildlife medical clinic, rehabilitation therapy, and much more.
It’s an exciting time to be part of the teaching hospital. A new $21 million addition for our oncology service should be completed by the end of next year. This expansion will allow us to treat more animals with cancer and continue advancing cancer treatment options through research.
You might be surprised how far animal owners travel to access the resources at the University of Illinois Veterinary Teaching Hospital. They come from all across the state of Illinois, from both coasts, and even other countries! For anyone who needs advanced or specialty veterinary care, I strongly encourage looking into the options available in Urbana. Thank you for your continued support, and I look forward to seeing many of you in the clinic over the next few years.
— Dr. Drew Sullivan, Medical Director
